Venous Ulcer of Lower Leg
History:
60-year-old woman, ambulatory, smoker, no diabetes, no history of surgery or trauma to the leg, no other significant medical history. She developed a small ulcer without any known cause or trauma above the medial ankle. This progressively grew in size over 3-4 months. She presented with a very painful, malodorous ulcer
Findings:
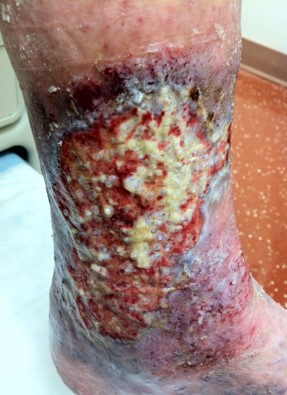
The ulcer at presentation at time of presentation 09/2012 Age is 3-4 months
Diagnosis:
Diagnosis: Venous leg ulcer. Diagnosis is made by history and clinical exam and ulcer characteristics. Arterial disease was ruled out with clinical exam and vascular studies with ultrasound
Differential Diagnoses:
Workup Required:
- Color duplex ultrasound scanning of lower extremity veins with Valsalva or proximal compression
- ABI/PVR or ultrasound for arterial flow
- Deep swab culture
Plan:
The plan included regular visits to the wound center for wound care and compression. Initially, the visits were twice weekly to monitor the response of ulcer, control drainage, and monitor the effect on ulcer pain. Once pain and drainage improved and the ulcer started showing new epithelization frequency of visits was once a week. Throughout treatment sustained compression was applied to the foot, ankle, and whole leg with multilayer compression bandaging once or twice weekly. The patient was educated on how to care for the ulcer and apply a commercial multilayer compression bandage system and she was able to do that at home
Expertise Needed:
Treatment:
- Wound care involved gentle cleaning of ulcer and surrounding skin with gentle soap and water to remove loose debris/slough. Once ulcer pain was improved patient was encouraged to shower with soap and water on the ulcer prior to dressing change and application of a new compression bandage. The ulcer bed improved with compression and drainage control, with resolving of the fibrin and slough in a few weeks. Debridement was not needed. The ulcer was treated with topical antibiotic ointment, non-adherent petroleum-based dressing, covered with an absorbent dressing, and then multilayer compression bandage to cover foot, heel, ankle, and all of lower leg. In the case of this patient, any other dressing would cause pain, so the dressing above was continued as it was comforting to the patient and allowed moist wound healing and progressive epithelization. At the time the ulcer was almost 90 percent healed the patient was referred to a vascular surgeon and underwent vein ablation in the same leg. Soon after the ulcer completely healed. After the ulcer healed patient underwent additional vein ablations in the same leg for treatment of venous reflux. She was followed for 5 years and did not have any ulcer recurrence
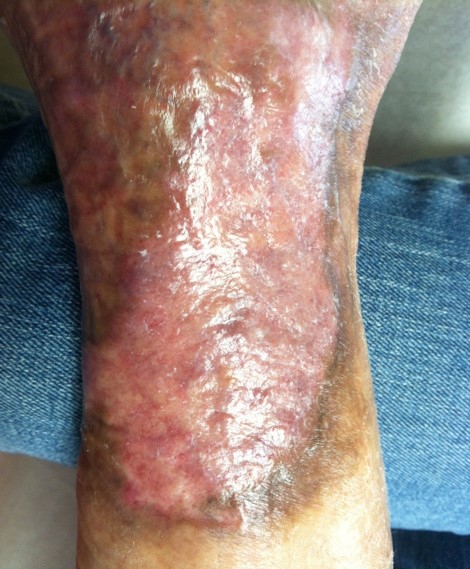
After 6 months of treatment the wound was completely healed.
Follow Up:
The ulcer continued to progressively epithelize. The treatment plan mentioned above and weekly visits were continued to monitor progress. The ulcer epithelized in 4 to 5 months except for a small area 4×4 mm in the lowest part of the ulcer recurred and would not close. The patient was referred to a vascular surgeon who did vein ablation in the same extremity. This area healed immediately after the vein ablation
The patient continued the multilayer bandage until the ulcer was covered with mature skin. At that time patient was transitioned to moderate to high compression stockings.
She required a few more outpatient vein ablations by a vascular surgeon. She was followed periodically for four years. The ulcer remained healed and there was no recurrence. She remained very compliant with wearing compression stockings daily

03/2013. Ulcer completely healed in 6 months.
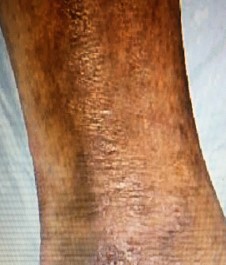
The ulcer remained healed 4 years later.

