Thumb Tip Amputation
An otherwise healthy 34-year-old male car mechanic sustained a crush injury to his left thumb tip after a car he was repairing slipped off of the jack crushing his thumb tip. He is right-handed, a non-smoker and has no other medical problems.
Findings:
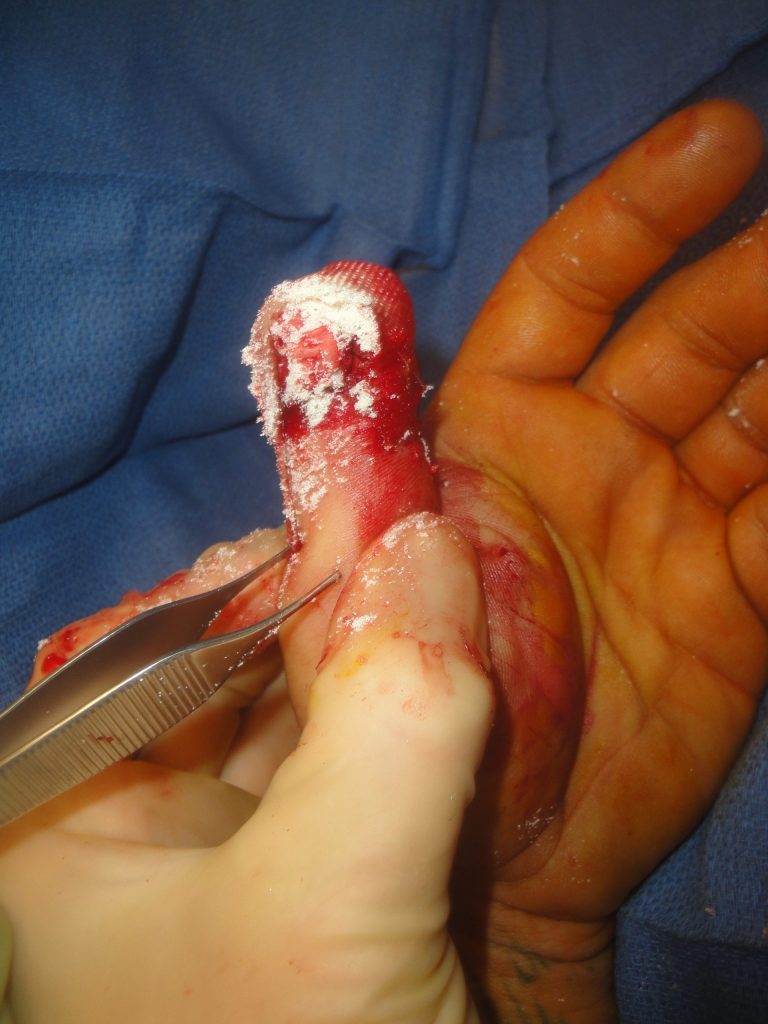
The tissues of the distal thumb tip were avulsed from the distal phalanx which had a fracture of the tuft leaving denuded distal phalanx bone protruding from the tip. The distal part was severely crushed and flattened.
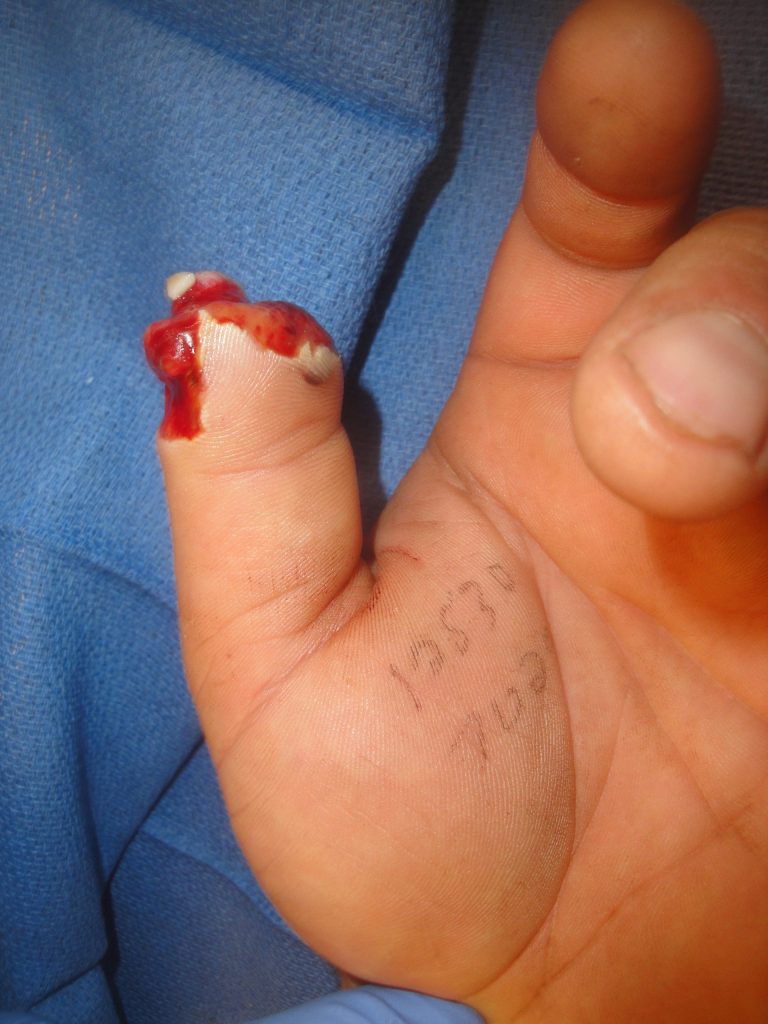
Fig.1. Left thumb amputation wound
Diagnosis:
Differential Diagnoses:
Workup Required:
Plan:
Initial management of most distal fingertip injuries with tissue loss can be managed with a copious application of a hydrogel and then referred to a hand surgeon for more definitive treatment. Various treatment options are available and should be specifically tailored to the patient’s vocation, avocation and anticipated hand use.
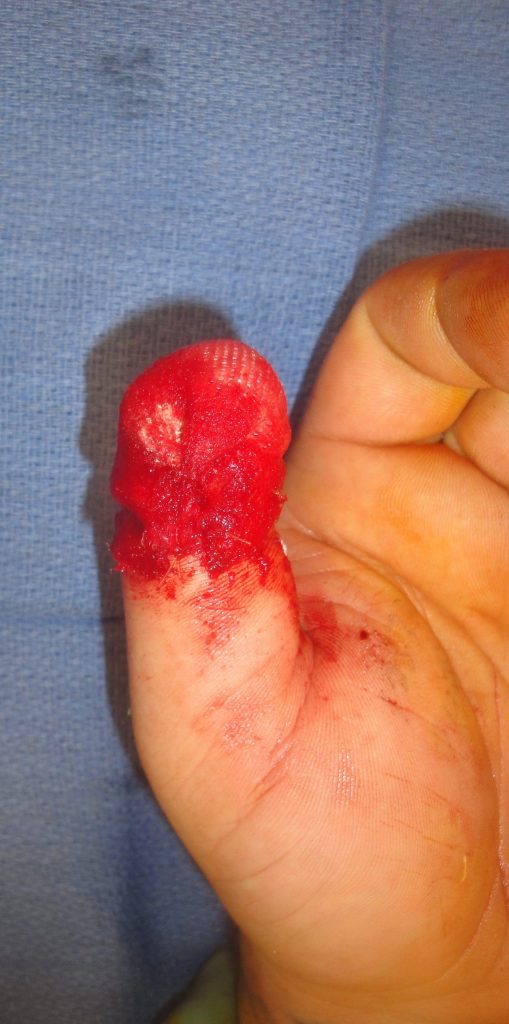
While topical wound management can be performed with serial hydrogel dressings alone it is unlikely to produce a durable stable coverage of the protruding bone. The addition of an Extracellular Wound Matrix device was been shown to be a relatively painless method to manage such wounds provide the patient has the time to allow for the constructive remodeling healing.
Expertise Needed:
A hand surgeon with particular interest in soft tissue reconstruction should assess the patient. Knowledge of the use of Extracellular Matrix Wound Healing Devices is desired as these devices facilitate healing through a process termed “site-specific constructive remodeling”- promotion of the formation of more normal tissue which often minimizes scarring. This M-2 macrophage directed healing is highly desirous in treating a seriously injured hand.
Fig. 2. ECM on thumb tip
Treatment:
Follow Up:
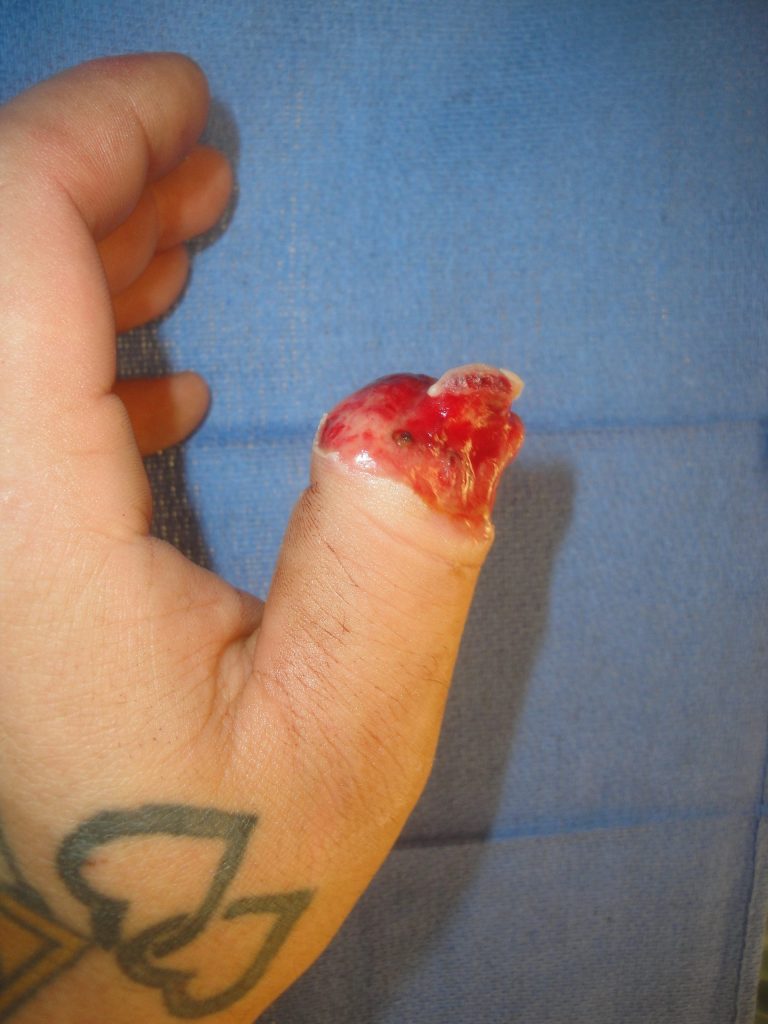
The fingertip had progressive healing but at 2 months-an additional 10 mg of MicroMatrix UBM-ECM powder was applied and final healing was achieved at 3 months. Final photos were taken at 4 months post-injury.
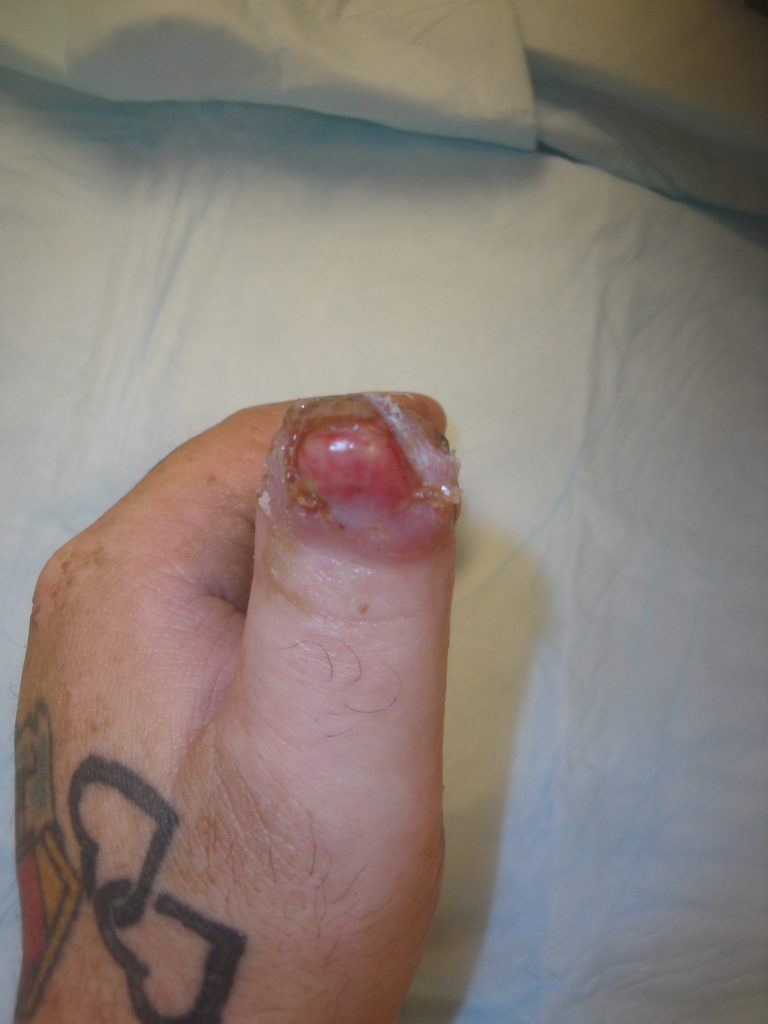
Fig.3. Thumb tip appearance at 2 months
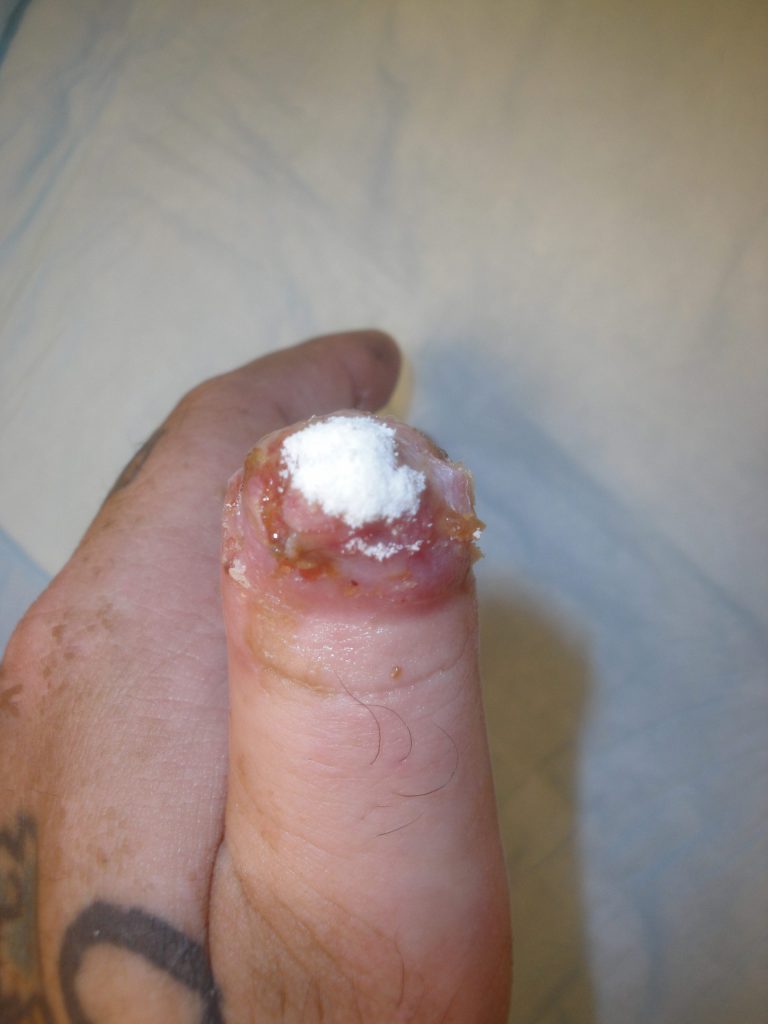
Fig.4. Additional placement of 10 mg UBM-ECM MicroMatrix powder at 2 months
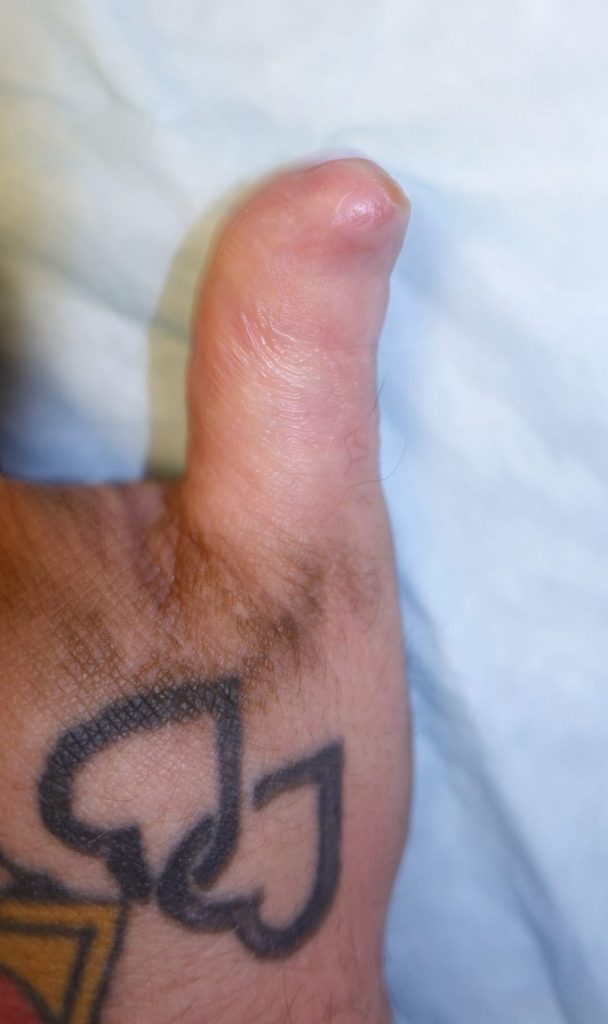
Fig.5a. Final left thumb tip appearance at 4 months post-injury.
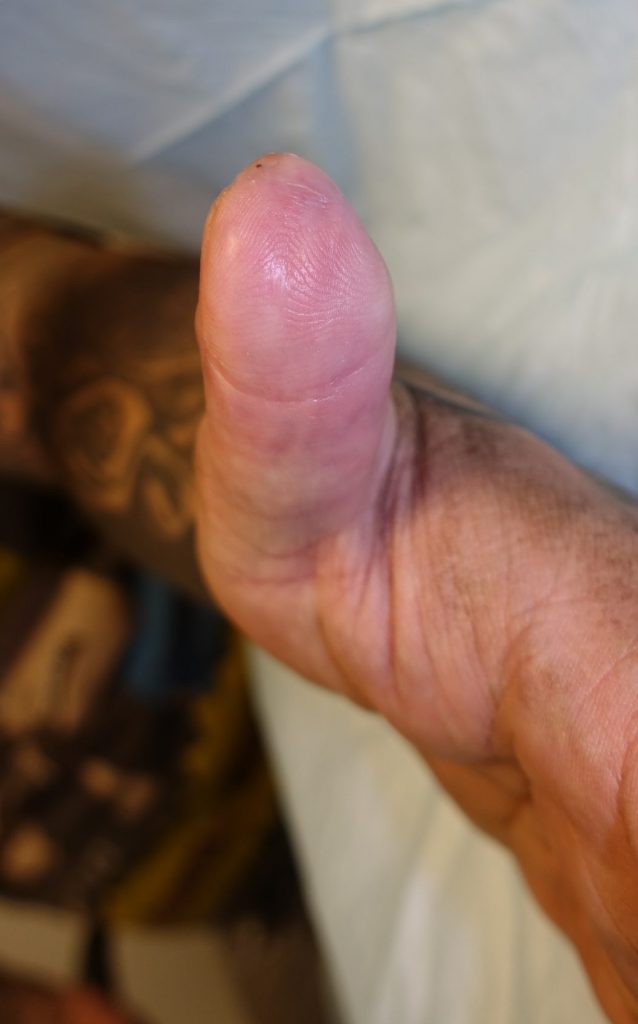
Fig.5b. Final left thumb tip appearance at 4 months post-injury.
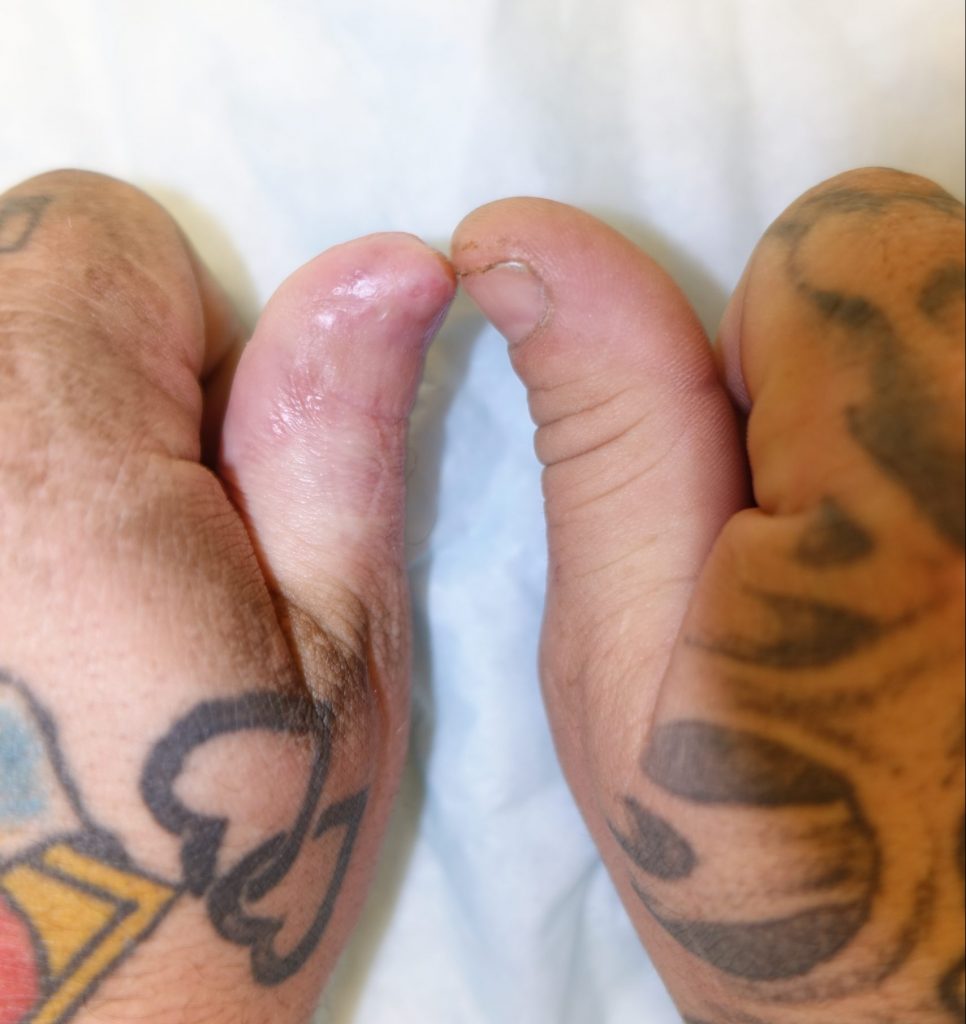
Fig.5c. Final left thumb tip appearance at 4 months post-injury.
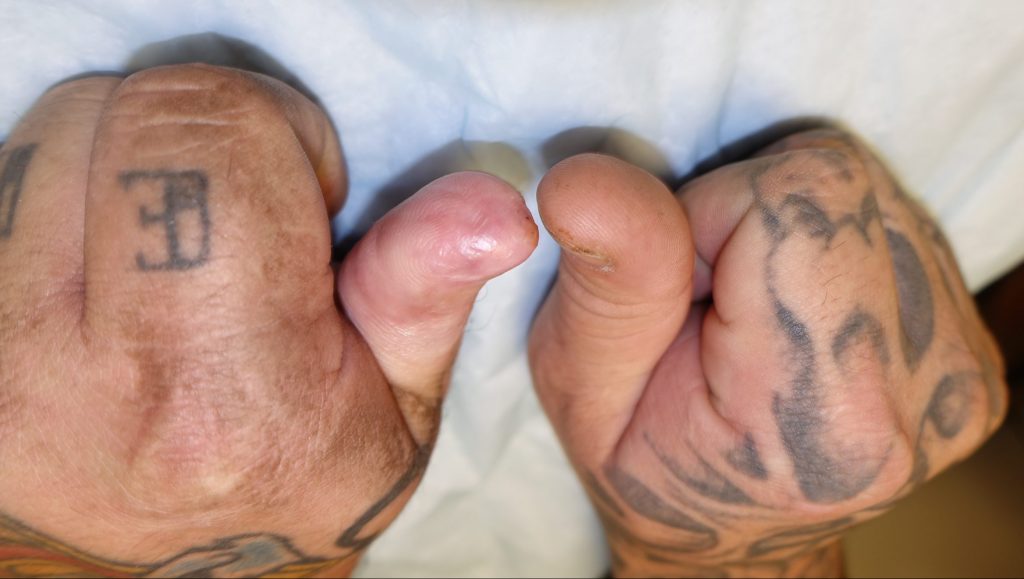
Fig.5d. Final left thumb tip appearance at 4 months post-injury.