Third degree burn in the face
History:
The patient is 85 years old lady, who collapsed against the side of the stove. Short period of unconsciousness. Previous cardiac infarction, medication for atrial fibrillation and hypertension. Lives alone with daily help.
Findings:
On arrival alert, no neurological deficits. 2.5% TBSA deep facial burn on the left side, Fig.1.
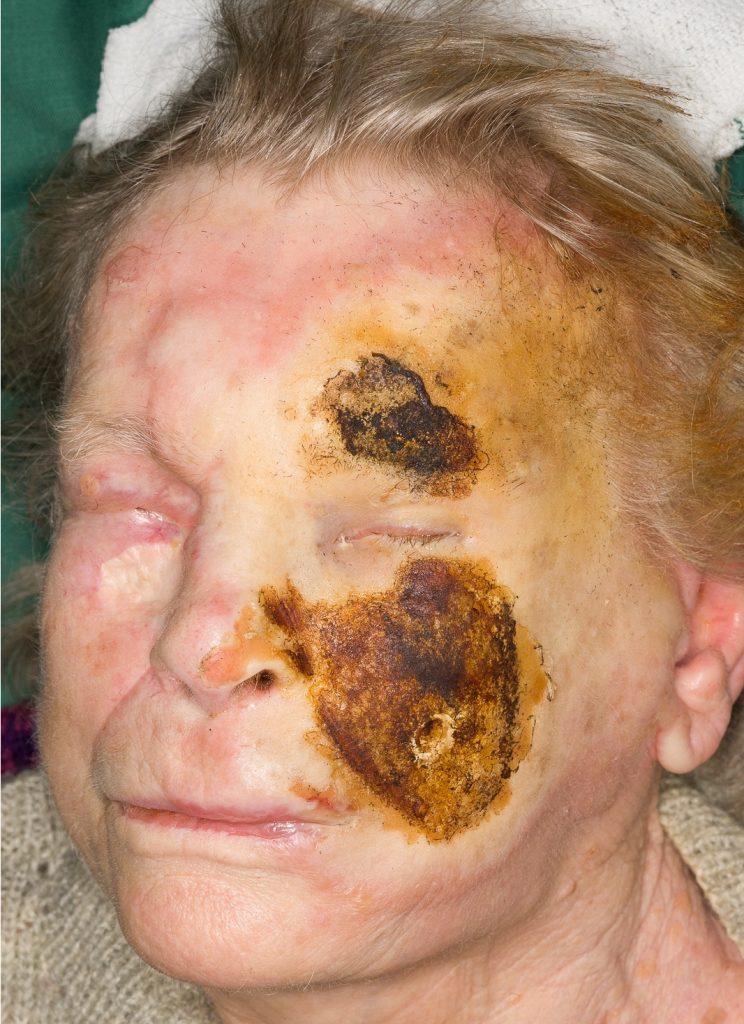
Fig.1. 3rd degree burns on the left cheek and brow regions. Deep 2nd degree burn with whitish color on the left side of the face.
Diagnoses:
Deep second and third degree burns on left side of face, 2.5% TBSA.
Differential Diagnoses:
No differential diagnoses related to burns.
Workup Required:
Ophthalmologist consultation needed: slight bulbar chemosis, no corneal affection, vision unchanged. Reason for collapse needed to be worked up.
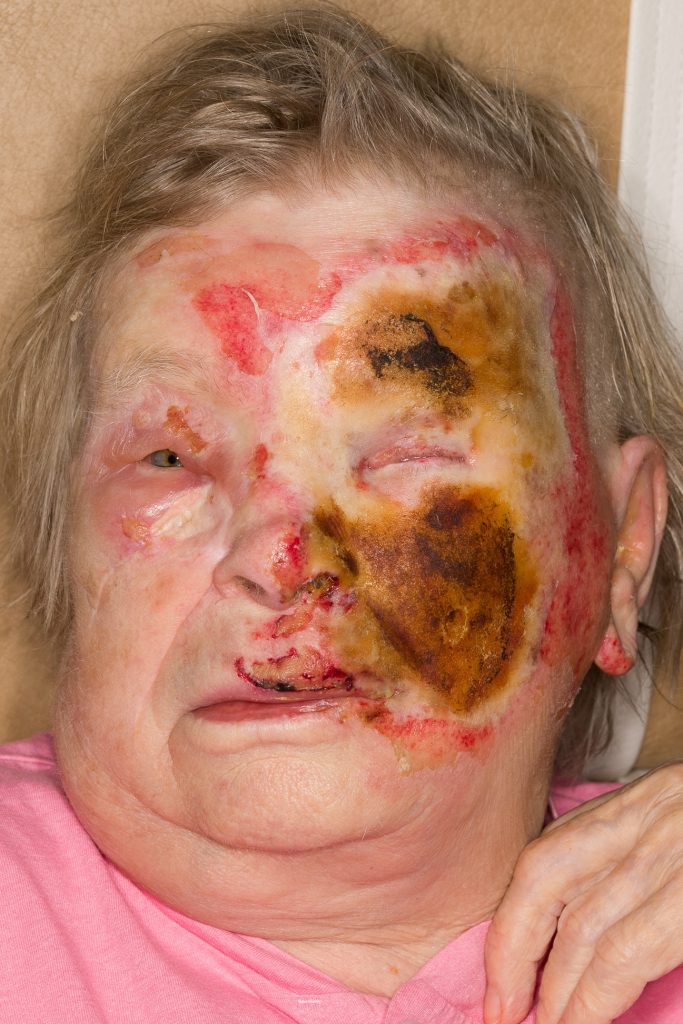
Fig. 2. Day 3 from injury. Demarcation of of the burn boundaries clearer, some deepening of the burned areas.
Treatment:
1) Waited for 3 days to observe the final depth of the burn, Fig. 2. Meanwhile use local antimicrobial cream ( silversulfadiazine).
2) Tissue sparing debridement was then done. Curettage or careful excision and hydrosurgery (Versajet®) of necrotic tissue. Coverage with allograft.
3) Second debridement after 4 more days and coverage with allograft, and plan skin grafting 3 weeks after burn.
4) Final coverage with full thickness skin graft, (defatted with hydrosurgery) from abdomen when wound bed is ready for graft take.
Expertise Needed:
Thorough knowledge of burn pathophysiology and wound healing. Expertise in burn surgery and burn reconstruction.
Day 7, second debridement, eye lids with scalpel, and rest of the wound area with hydrosurgery, Fig. 5.
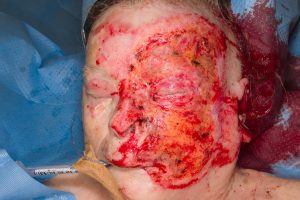
Fig. 5. Debridement eith knife and hydrosurgery.
Full thickness skin graft harvested from abdomen with scalpel and monopolar cautery. All fat was removed with scissors and hydrosurgery. Skin graft was sutured in place with monofilament sutures and Artiss® tissue glue was added under the graft to enhance the graft adherence. Tarsoraphy was performed. Donor site in the abdomen was closed primarily like in abdominoplasty. Tulle ointment gauze and compressing dressing were applied on the graft. The patient was extubated right after the surgery.
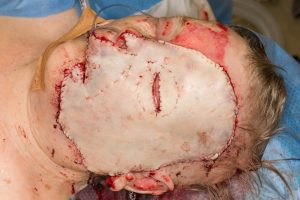
Fig. 6. Full thickness graft sutured to the face.
Follow Up:
7 days after skin grafting the graft take was almost complete. Darker bluish color around left nasolabial fold typical for full thickness skin (FTA) graft Fig. 7.
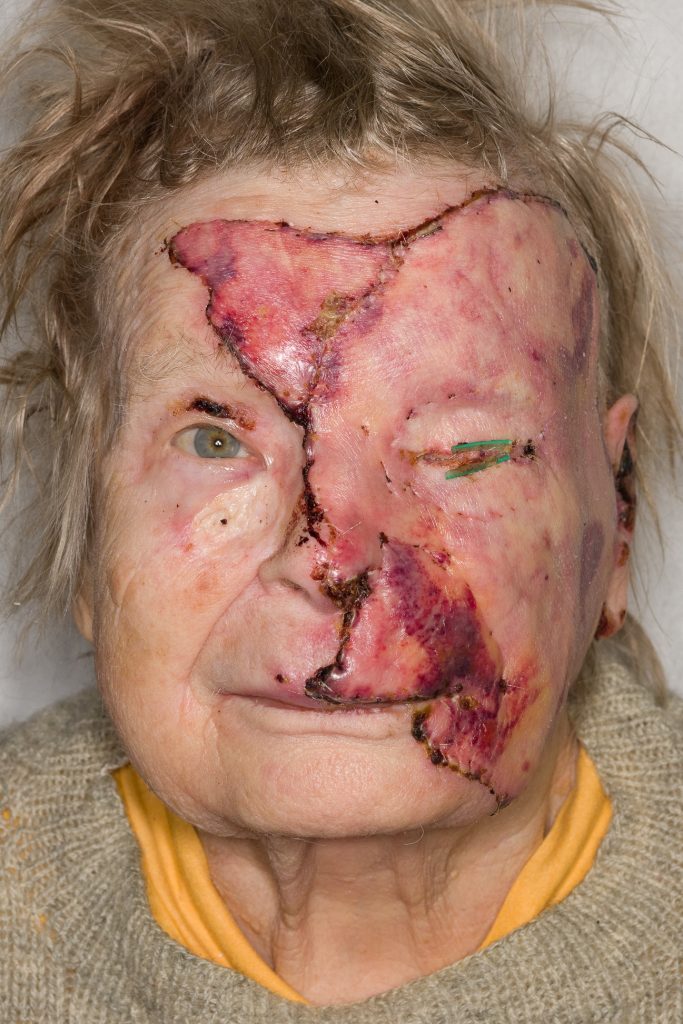
Fig. 7. One week after full thickness skin grafting.
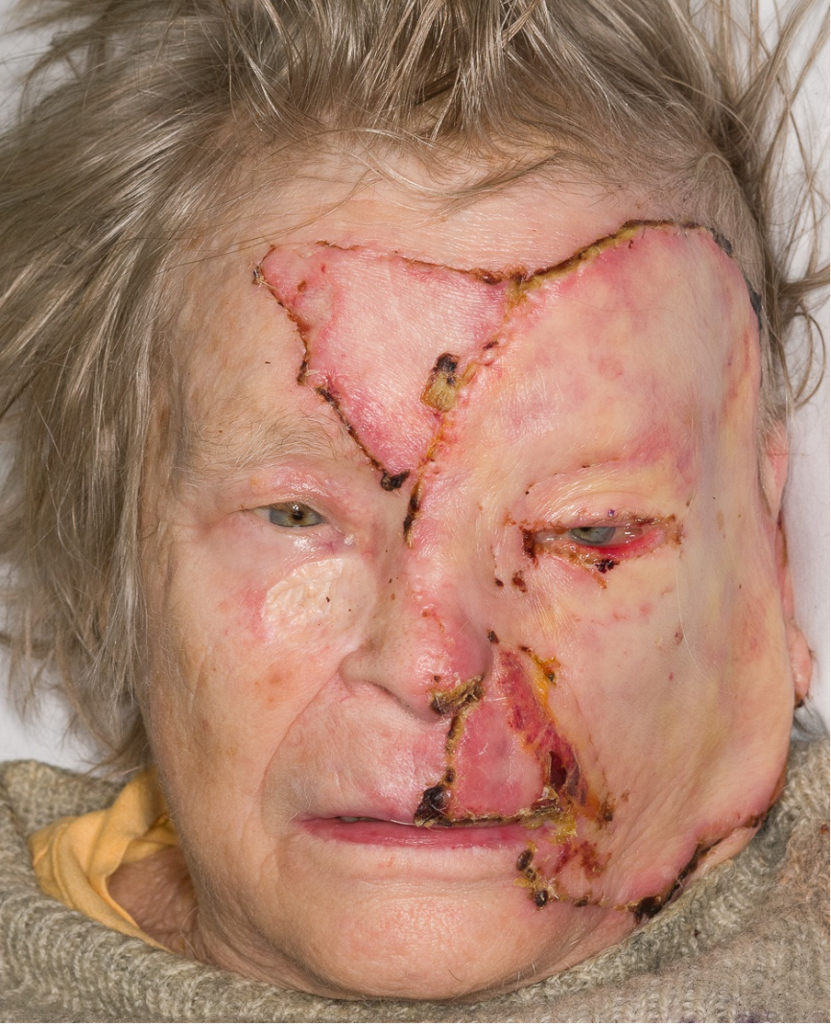
Fig. 8. Three weeks after grafting.
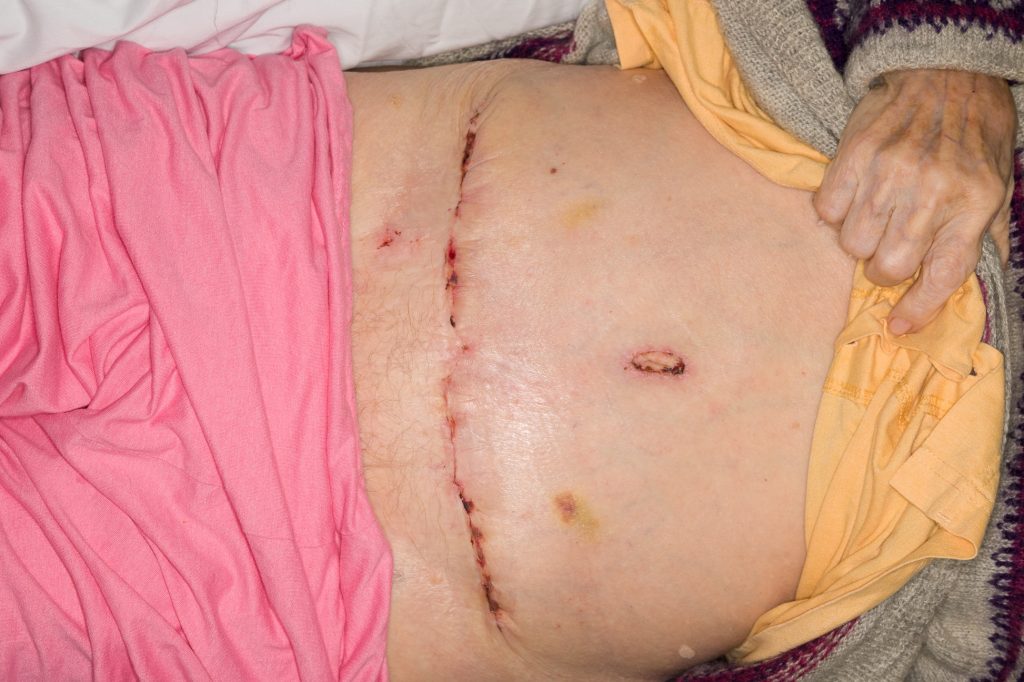
Fig. 9.
Directly closed donor site after three weeks.
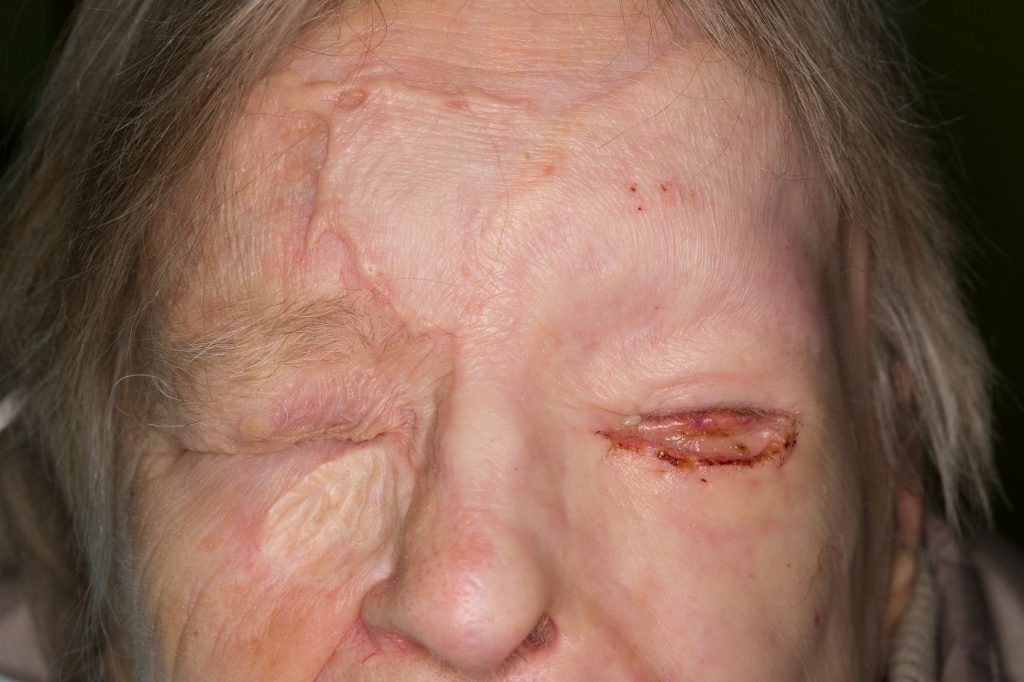
3 months after grafting the skin was supple, ectropion in the lower lid that was corrected with full thickness skin graft, Fig. 10 – 13.
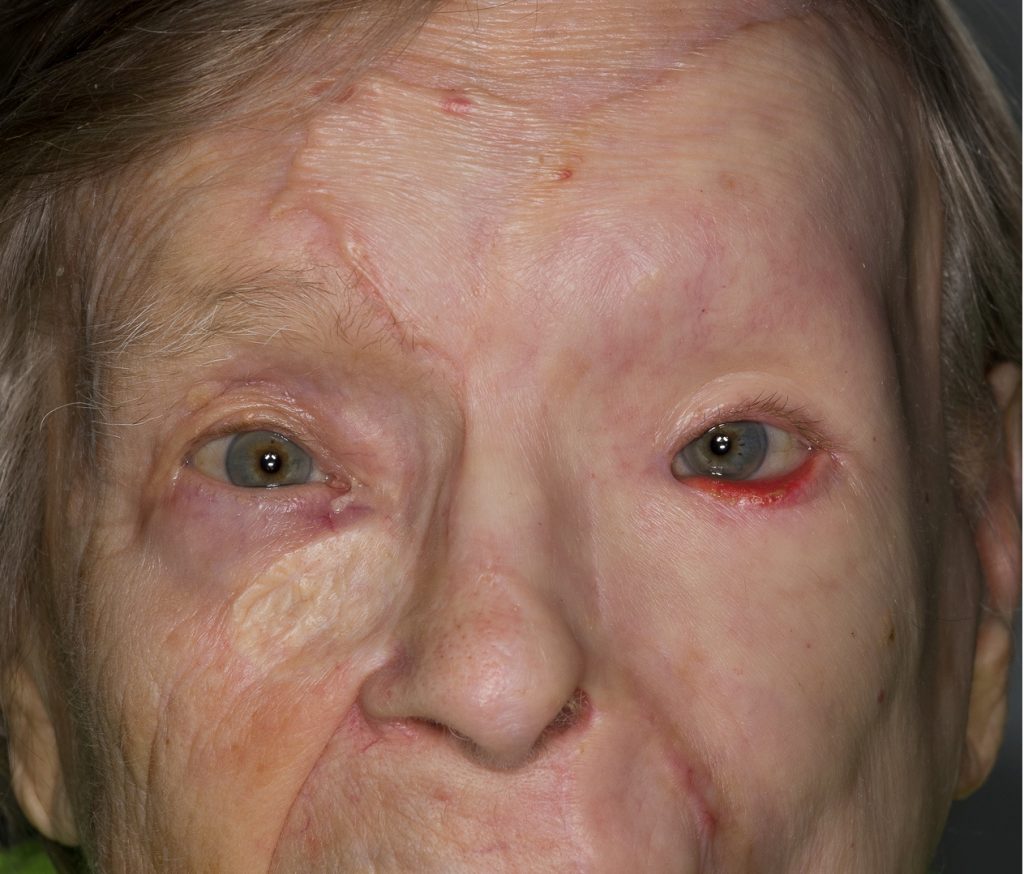
Fig. 10. Three months after grafting. Ectropion in left lower lid.
Fir.11. Full thickness graft harvested next to the abdominal scar. Skin graft from behind the earlobe has the best color match in face but this time the previous large graft was also from the same area with similar color.
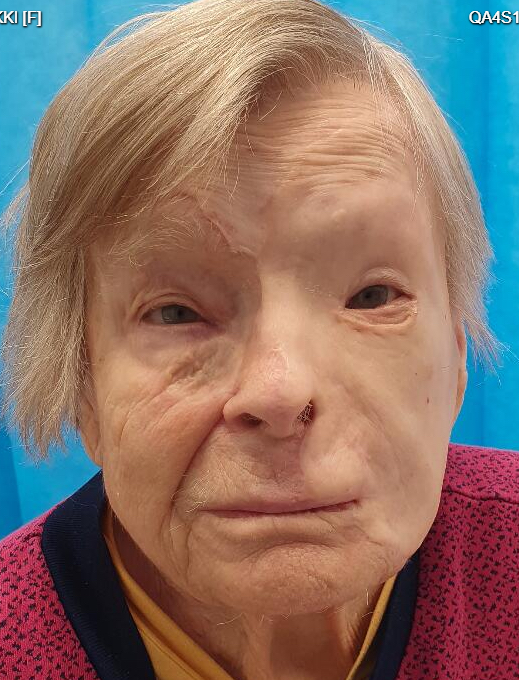
Fig.12. 6 months after injury. Final result. Some scarring in the lower lid but no ectropion.

