Large occipital scalp keloid treated with tissue expansion
History:
Patient is a 39-year-old male with a past medical history of Hypertension, Hyperlipidemia, and Atopic Dermatitis, who presented to the dermatology clinic with a five-year history of severe recurrent Acne Keloidalis Nuchae in his posterior scalp. His keloid was mildly pruritic, and was treated with 0.05% fluocinonide ointment, 0.1% cream, intermittent course of Bactrim and steroid injections, with no significant improvement. He expressed interest in surgical excision and was referred to the Plastic & Reconstructive Surgery Team. The patient avoided irritation or trauma to the area, but occasionally trimmed hair growth from the lesion. Family history was significant for Acne Keloidalis Nuchae of his father that improved with Bactrim treatment. Surgical history was also significant for inguinal hernia repair. He did not smoke.
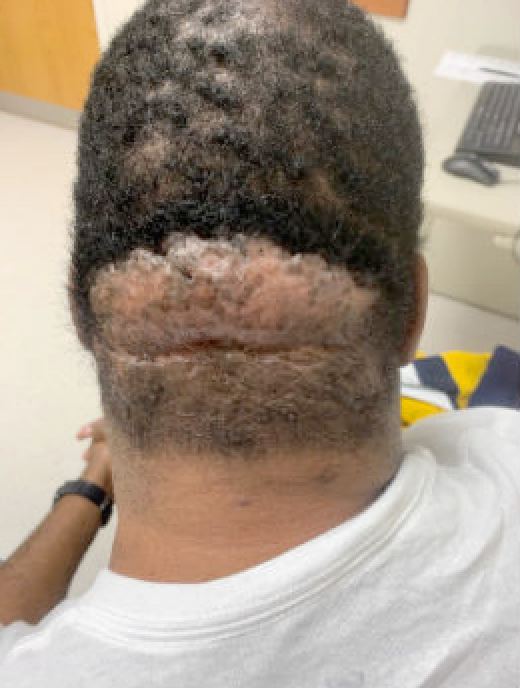
Fig.1.Photograph from initial consultation that showed the result of five-year progression of Acne Keloidalis Nuchae on posterior scalp.
Findings:
At evaluation, the patient was in no acute distress. He had a keloid involving the inferior occipital scalp that was approximately 12cm x 6cm. It was a well-defined, skin colored plaque, and 99% alopecic. Across the superior surface, there were several tufted hairs. It lacked pustules or significant erythema.
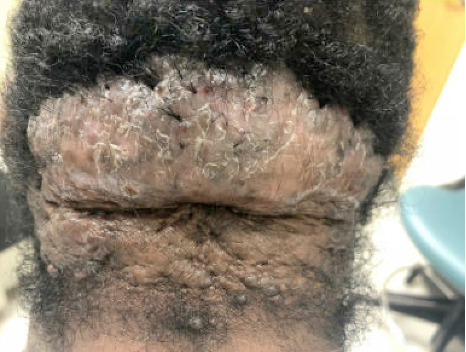
Fig.2. Picture in higher magnification from initial consultation depicting the result of five-year progression of Acne Keloidalis Nuchae on posterior scalp.
Diagnosis:
Severe, Acne Keloidalis Nuchae on Posterior Occipital Scalp
Differential Diagnoses:
Workup Required:
Plan:
The suggested method of treatment was full excision of the keloid with initial repair using a split thickness skin graft. This would remove the scarred tissue with potentially infected deep acne. Tissue expansion was to be considered upon sufficient healing.
Expertise Needed:
The patient had been treated by his dermatologist for 5 years with topical antibiotics and intralesional steroids. There had been temporary improvement, but overall the keloid had progressed. The patient was therefore referred to a plastic surgeon for excision and staged scalp reconstruction.
Treatment:
5/29/2020
Patient was administered IV antibiotics, general anesthesia, and intubated prior to surgery. He was placed prone to perform excision and skin graft. A measurement of the keloid on the posterior scalp was taken on a template, which was transferred to the left posterior thigh to determine the skin graft size. A tumescent mixture of saline and lidocaine was injected into the tissue and periphery followed by a full thickness incision, in which the skin and underlying subcutaneous tissue was dissected. The keloid was sent for pathological evaluation. The wound bed was prepared for skin grafting and irrigated with saline. The Zimmer dermatome was set at 14/1000 of an inch and we used the 4-inch guard. The skin graft was meshed 1 to 2 and applied to the posterior scalp. It was sutured in place and trimmed as needed. Quilting sutures were used to ascertain adherence of the skin graft to the wound bed. An interface dressing was placed directly over the skin graft site, followed by the sterile Reston foam and Fine mesh gauze on the sticky ends. The grafting site was treated with a Tegaderm, ABD and an Ace wrap.
After several clinic visits, the patient requested another reconstructive procedure to repair the alopecia on his posterior scalp. The wound demonstrated sufficient healing, and no keloid reoccurrence, which permitted tissue expansion.
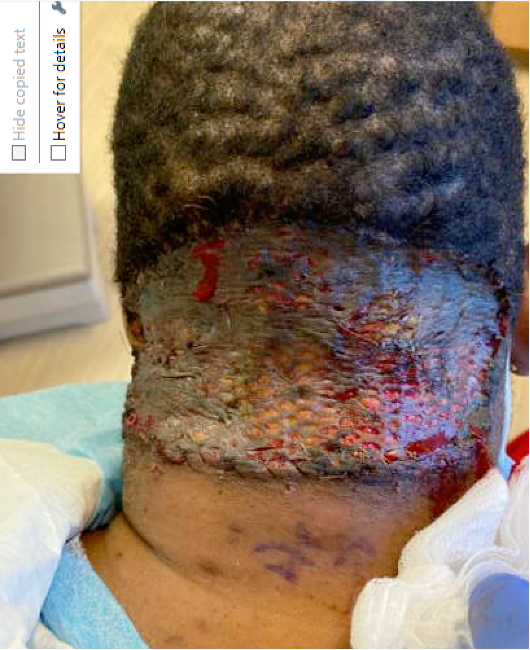
Fig 3.Two weeks post-operative posterior scalp skin graft.
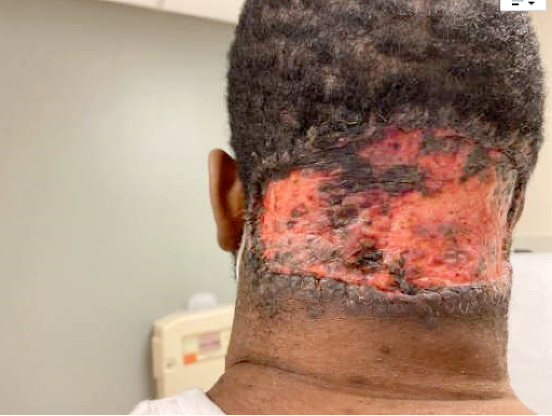
Fig.4. Four weeks postop. demonstrating healing of posterior scalp excision site with skin graft.
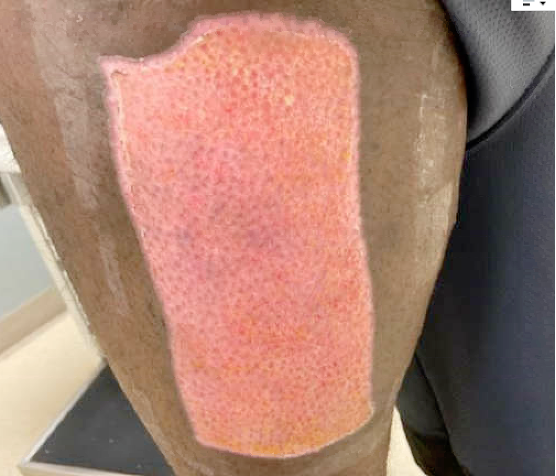
Fig.5. Left posterior thigh donor site at 4 weeks.
We injected our tumescent mixture deep to occipital scalp in the intended location of the tissue expander and dissected to the subgaleal plane. A subcutaneous tunnel extending towards the right mastoid area was created. We then copiously irrigated out the soft tissue cavity with antibiotic and Betadine mixtures. A flat, kidney-shaped Softspan tissue expander 14 x 9 x 4 cm was selected and placed in the subgaleal space with a 10inch-French flat JP drain secured in place. After closing the skin at the deep tissue and dermal layers, we percutaneously accessed the tissue expander and then injected it with 70 mL of sterile injectable saline. Dermabond and an appropriate gauze wrapping was applied to the surgical site.
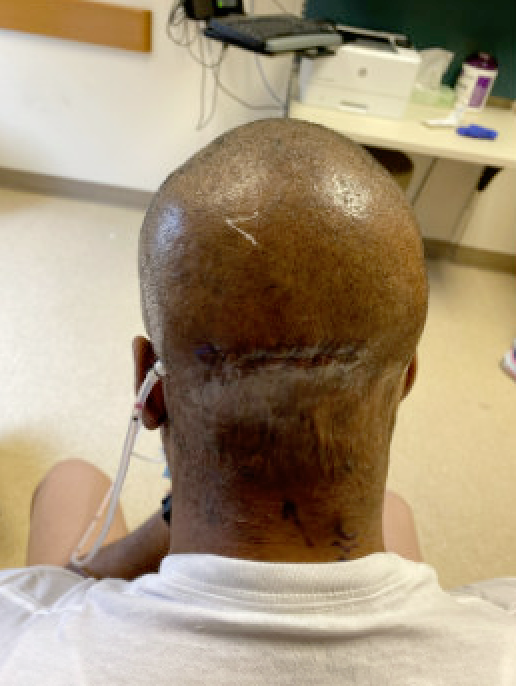
Image 6. Subsequent post-operative clinic visits to begin tissue expander injections.
After the tissue expander was filled to 410mL over the course of six months, the final stage of removal could take place. This began with dissecting through skin and subcutaneous tissue and emptying the saline from inside. After freeing the expander from surrounding tissue, scalp advancement took place with exposure of the tissue expander injection port behind the right ear. Once the tissue expander and port were removed, the subgaleal plane was undermined anteriorly and laterally to further scalp advancement to allow for Galeal scoring afterwards. The area of alopecia was excised and measured 12.5 x 8 cm. A 10Fr flat drain was placed behind the left ear with 10mL of FloSeal injected in the cavity. The scalp was advanced posteriorly with sufficient tautness. Closure took place at both the deep and skin layers, with the application of Bacitracin and Xeroform, gauze, and head wrap to the incision.
Follow Up:
The patient had his post-operative follow up one and six weeks after the final surgery for tube inspection. Reconstruction site demonstrated sufficient healing and void of hypertrophic scarring or keloid formation. He was very happy with result. Monitoring will continue, alongside recommendations for scar massage and sunscreen use.
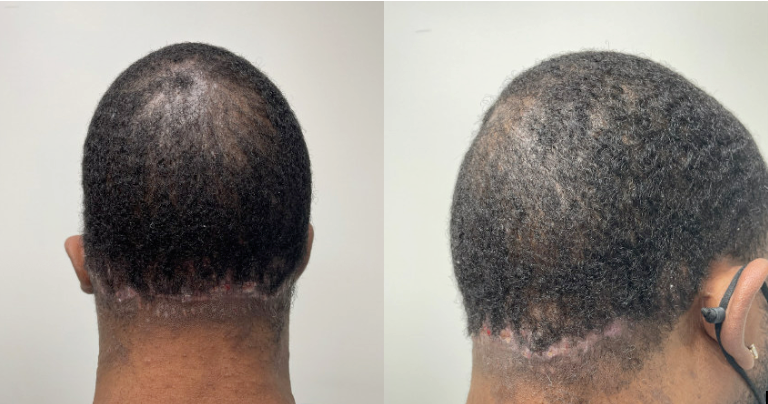
Fig . 7. Result depicting week 6 post-operative removal of tissue expander and advancement of posterior scalp.. Reconstructed site was free of hypertrophic scarring or keloid formation. Natural-appearing hairline was maintained.

