Laceration/tear in upper arm in patient with fragile skin
History:
An 86-year old female multi-morbid patient was admitted in our hospital for a planed open carpal tunnel release operation. The patient had several heart diseases (Heart failure, aortic valve stenosis, mitral valve stenosis, atrial fibrillation) and she also had had multiple operations done on her (total hip replacement surgery on both sides, total knee replacement surgery on the left) without wound healing disturbances. During the physical examination the patient had very thin and fragile skin.
Findings:
At the end of operation while removing the sterile operation covers we noticed a circular laceration, from pressure and shear, caused by the rubber cuff of the tourniquet. Only epidermis and part of the dermis were injured. The finding was photo-documented.
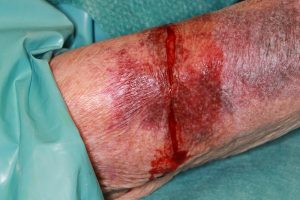
Figure 1. Shows a circular laceration/tear to the upper arm when the tourniquet was removed.
Diagnosis:
Circular superficial skin laceration of the right forearm in a patient with very fragile-skin.
Workup Required:
The patient was made aware of the possible complication and further operation if needed in case of disturbances during healing. The status of TDaP-Immunization, allergies, history of wound healing disturbances should be explored with the patient.
Plan:
Repair of the laceration under local anesthesia.
Expertise Needed:
Plastic surgeon or Hand surgeon.
Treatment:
In this case the patient had already received a brachial plexus regional block (the procedure could also be done in a local anesthesia). The wound was irrigated thoroughly with sterile saline and the depth and involvement of surrounding structures were examined. No functional structures were injured and underlying fascia was intact. Picture 1 demonstrates the thin fragile nature of the patient’s skin due to age-related atrophy of epidermis and dermis. A conventional two layer wound closure could not be done. The wound was therefore closed with two dermal rows of 5-0 Vicryl sutures subcutaneously and a 5-0 Monocryl running locking suture. Consequently followed by application of Dermabond skin adhesive to increase strength and reinforce the wound edge (Picture 2). A dry wound dressing as well as a dorsal splint for 3 days was applied to reduce involuntary movement and tension on the wound.
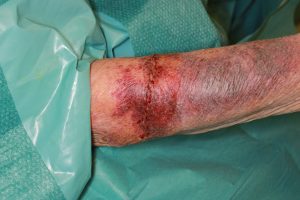
Figure 2. Shows the wound after suture and wound adhesive closure.
Picture 2
Follow Up:
The patient was observed and the wound dressing was changed daily for 4 days. The patient could be discharged on day 4 after the operation without any wound complications. At the follow up after 10 days the wound showed good healing without complications.

