Radiation Ulcer of Breast
History:
The patient is a 65-year-old woman who presented for initial evaluation on 2/14/22 for a nonhealing wound present along left mastectomy surgical incision.
She was diagnosed with left breast carcinoma in June 2019 and treated with lumpectomy, chemotherapy from August 2019 to January 2020, and 19 radiation treatments from February to March 2020. Cancer reoccurred in August 2021 with no evidence of metastatic disease. In October 2021 she underwent bilateral mastectomy and left axillary dissection, and she deferred reconstruction. The overall stage was rpT1c pN0 M0. She had a drain in place on the left side for 9 weeks, which was removed on 11/29/21 secondary to MSSA infection. She was started on chemotherapy with Taxol on 1/4/22. She developed a fever the next week, with tenderness and redness to the left chest wall site with an opening in the incision and drainage. She was seen by her oncologist on 2/2/2022 who noticed two areas of wound dehiscence with purulent drainage along the left chest wall surgical incision. The wound was cultured and she was referred to an infectious disease specialist and treated for mastectomy site cellulitis with IV daptomycin and PO Keflex for treatment of MSSA culture. The infection improved, however, however the wound still remained open and she was referred to the wound center by the infectious disease specialist. She was seen in our wound center for an initial evaluation on 02/14/2022.
Ulcer at initial visit
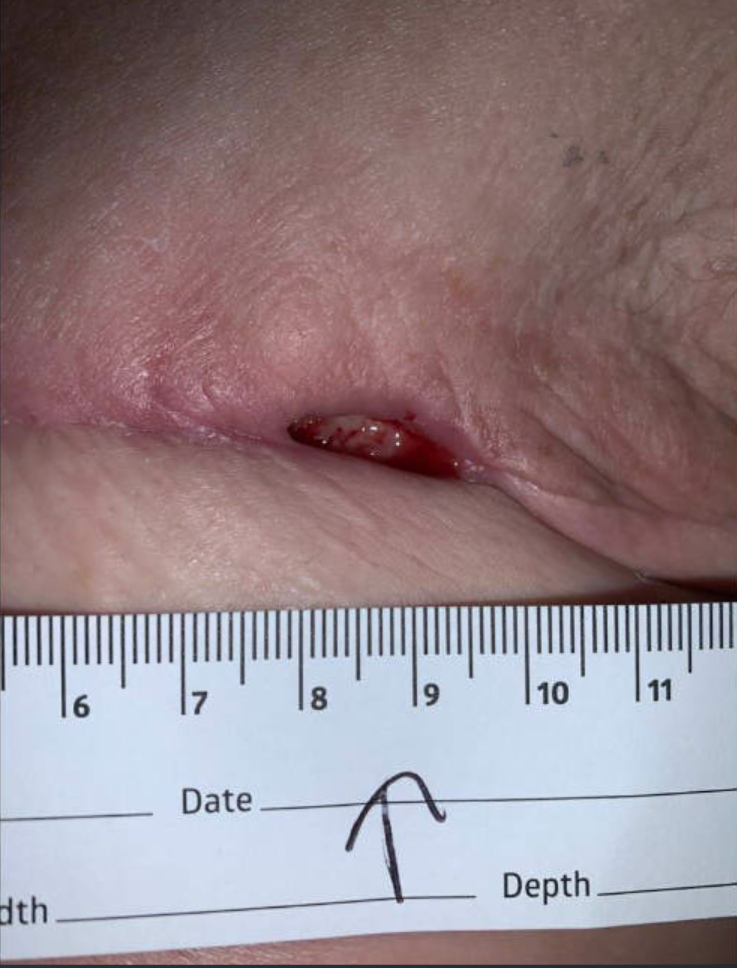
Findings: On 2/14/22
Dressing Appearance intact (gauze was removed. Pt’s husband explained that he removed the aquacel ag already.)
Drainage Amount large
Drainage Characteristics/Odor yellow; serosanguineous
Base other (see comments);slough (white/yellow)
Peri wound scarring; indurated
Edges rolled
Wound Length (cm) 0.5 cm 02/14/22 1021
Wound Width (cm) 1.8 cm 02/14/22 1021
Wound Depth (cm) 0.5 cm 02/14/22 1021
Wound Surface Area (cm^2) 0.9 cm^2 02/14/22 1021
Wound Volume (cm^3) 0.45 cm^3 02/14/22 1021
Undermining [Depth (cm)/Location] 1.5cm undermining from 3-9 o’clock 02/14/22 1021
Left chest wound/ulcer is open at the incision line, there is epibole at the edges and underminig of 1.5cm from 3-9 o’clock. Ulcer bed is covered with yellow slough, fatty tissue. There is A large amount of yellow serosanguinous odorless drainage. Periulcer area is scarred, there is no outstanding warmth, erythema, mild tenderness.
There is no induration at left axilla, no crepitus or fluid palpated.
Diagnosis:
Ulcer left chest along healed surgical incision following mastectomy more than 7 months earlier and nonhealing was most likely secondary to late effects of radiation therapy. There were no signs of infection on the initial visit or during follow-up visits
Differential Diagnoses:
Workup Required:
Wound biopsy to r/o cancer recurrence
Wound cultures; DNA and Biofilm cultures preferred, otherwise deep swab cultures
Full hematology and chemistry panels
Chest x-ray
Plan:
Expertise Needed:
Treatment :
Initial Visit: The goal was to start topical antimicrobial ulcer therapy, debridement of devitalized tissue and moisture-balanced wound environment to assist in healing. There were no signs of local infection but there was slough covering 100% of the ulcer base, a large amount of creamy serous drainage, and rolled indurated edge Epibole) with 1.5 cm undermining along half of the edge
Ulcer treatment included cleaning well with Vashe ( pure hypochlorous acid which is noncytotoxic with a skin-friendly neutral pH). The open area of the ulcer was packed with MeSalt dressing as a debriding agent, and covered with an absorptive layer and foam. The patient and husband were taught how to do ulcer care and wound dressing daily
Week 2 follow-up: The ulcer was largely unchanged. Treatment included gentle sharp debridement using a curette to remove the slough. The same ulcer care and dressing were continued with a plan for the husband to do daily ulcer care at home. The decision was made not to excise the rolled edge because of the risk of making a larger ulcer in the skin compromised by radiation which potentially can take a long time to heal. A decision was made to wait and see if decreasing the slough and fibrin from the ulcer bed will allow the edge to attach to a healthier granulated wound bed thereby initiating epithelial migration.
Although at this time starting HBOT as an adjunct treatment would benefit the ulcer it was decided to wait until the patient finished chemotherapy with Doxorubicin. It was discussed with the patient that we will consider risk vs benefit and keep her chemotherapy as a priority and we will manage the ulcer with local ulcer care as the ulcer was stable w/o any sign of infection.
Week 3: the ulcer still had a build-up of slough with size largely unchanged. The edge was still rolled in and indurated however it had started attaching to the wound bed and a thin rim of new epithelization was noticed where the edge had attached. At this time sharp debridement with a curette was done to remove the slough. The topical was changed to cadexomer iodine on the ulcer bed to prevent a build-up of slough/biofilm or minimize it. The ulcer was covered with an absorptive dressing and protective foam. Skin prep was used under the adhesive for protection of the periulcer skin as irradiated skin can easily get irritated. The rolled ulcer edge or epibole was not debrided or excised to minimize the risk of developing a larger nonhealing ulcer in the skin that was compromised because of radiation. The patient continued daily wound care at home
Week 4: The wound edge started showing attachment to the ulcer bed along a greater area. There was still a build-up of fibrin/slough in the ulcer bed but was decreased and thinner. This was removed by debridement using a curette revealing a pink ulcer base. The rest of the treatment remained the same
Week 8 to week 14: Patient visit frequency to the wound center was changed to every 3-4 weeks. The ulcer edge became attached to the ulcer base all around and the undermining resolved. The drainage was decreasing however there was still a build-up of slough on the ulcer base. Gentle debridement of the slough was done during the wound visits twice during this time. The patient with help of her husband continued the same wound treatment at home however frequency was changed to every other day wound care and as needed
NOTE: The patient finished chemotherapy with Doxorubicin in week 11 but wanted to wait to start HBOT. The ulcer made some progress until week 11 but then stalled.
Week 14 to week 21: The ulcer had very little drainage so the treatment was changed to collagen-based dressing on the ulcer bed to minimize the slough. The wound did show progress with more epithelization however the progress was very slow.
The patient agreed to start HBOT week 21
Week 21 to week 26: Patient completed 30 HBOT treatments. The ulcer was completely epithelized by week 24 and completely healed by week 26
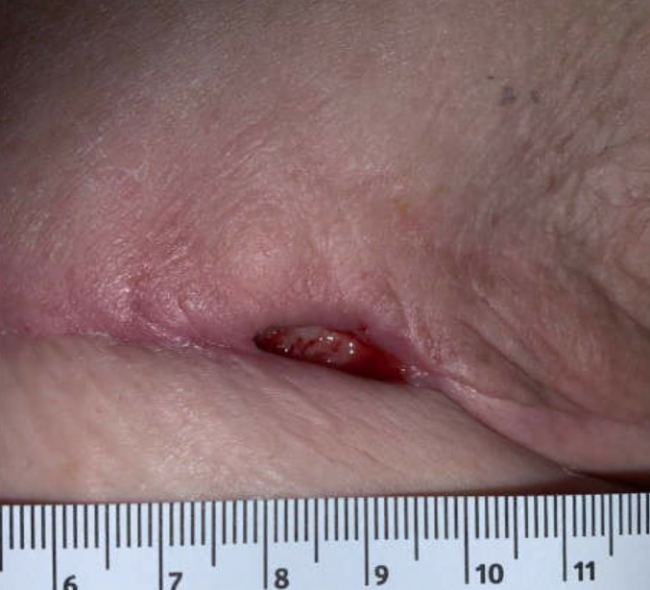
Ulcer at initial presentation
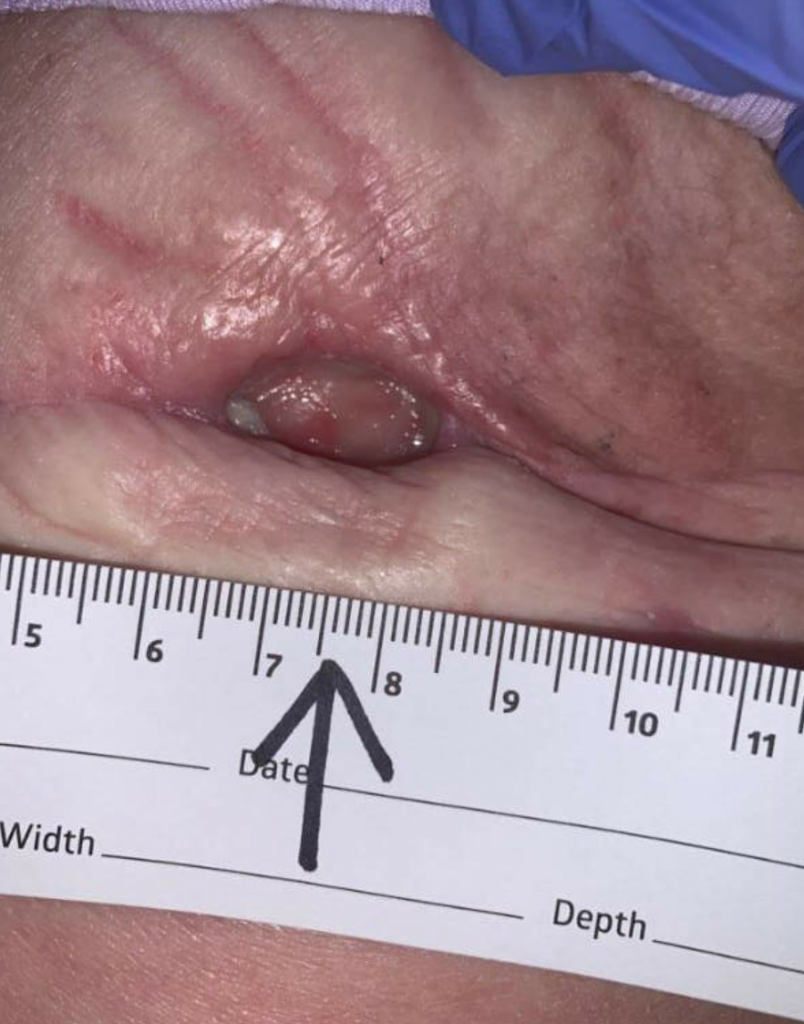
Ulcer at 3 weeks follow up
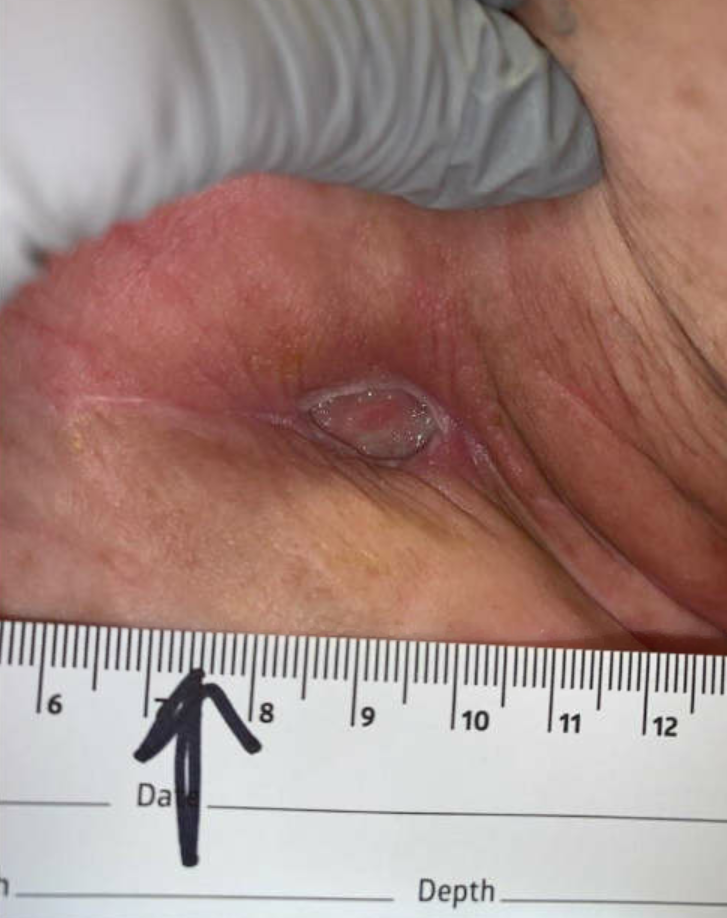
Ulcer at 14 weeks follow up
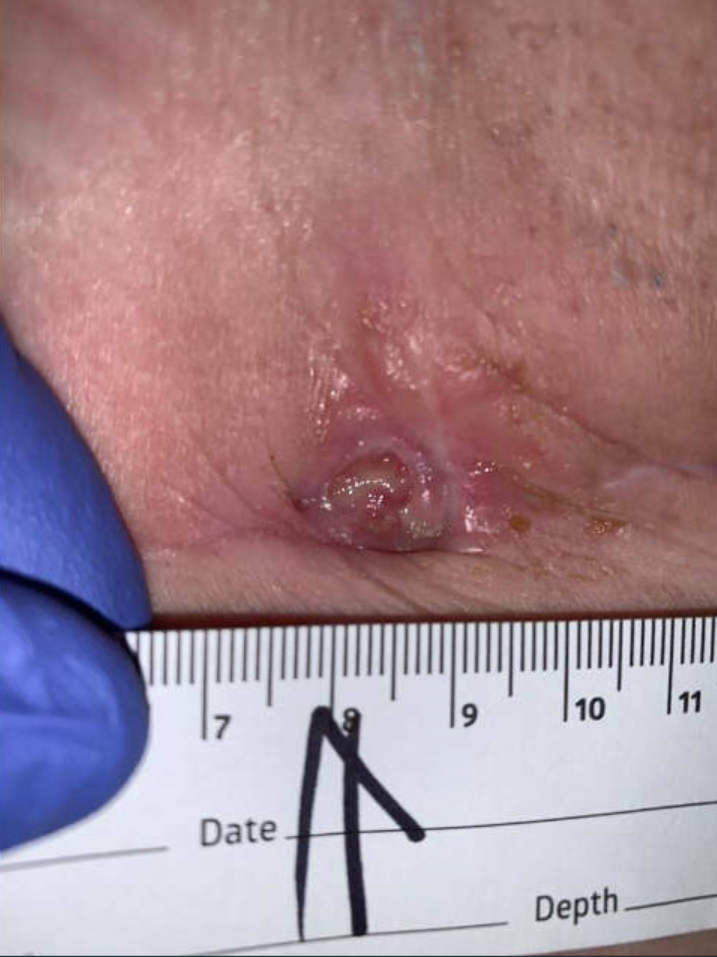
Ulcer at 21 weeks – HBOT started
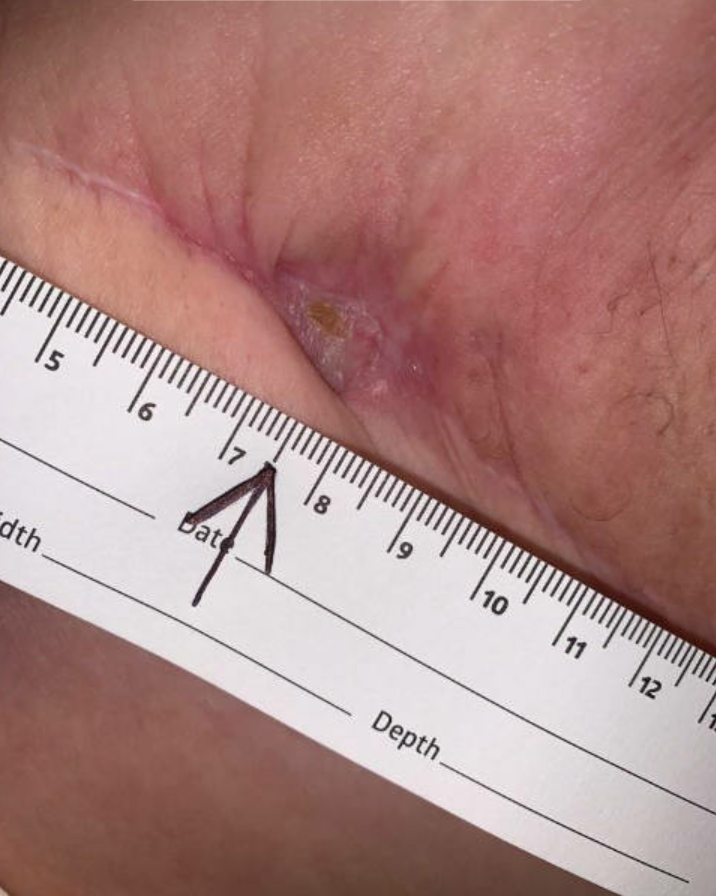
The ulcer healed after completing 30 HBOT treatments
Discussion:
The ulcer healed after completing 30 HBOT treatments. The HBOT was thought to facilitate healing by stimulating angiogenesis, improve tissue oxygenation and decreasing tissue fibrosis. It was also thought that HBOT helped increase stem cell mobilization.
Follow up:
The patient was discharged from the wound center after the ulcer healed.
The patient will continue to follow up with her oncologist.

