Open Ankle Wound with Exposed Orthopedic Hardware
This 80-year-old male weighing 475 pounds (BMI= 64) fell at home while getting out of his bathroom shower. Due to his large size, Emergency Medical Services had to cut him out of his bathtub where he had been trapped for several hours. He was hospitalized and cared for by the Orthopedic Service for 1 month prior to consulting the Plastic Surgery service for treating his open right ankle wound
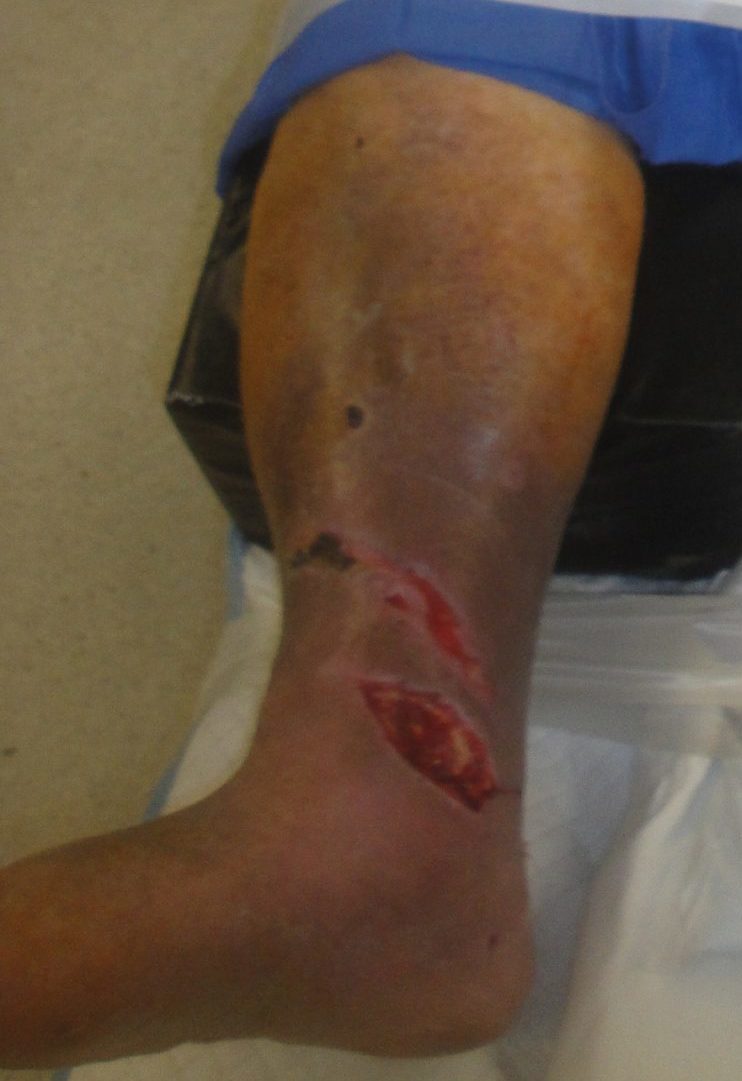
Fig.1. Patient with open right ankle wound
.Initial wound management with NPWT- note the hydrocolloid dressing was being used to protect the fragile venous stasis ulcer prone skinDuring this admission he had been treated twice for his acutely fractured ankle. Initially it was managed with both internal and external ankle fixation but 1 week later it was converted to total internal fixation after he refractured it while getting up and trying to ambulate on his own. His ankle wound had been managed with negative pressure wound therapy by the Orthopedic Surgical service prior to consultation
In addition to being an octogenarian, he had asthma, COPD, depression, anxiety, type 2 diabetes, hypertension, hyperparathyroidism, osteoporosis, psoriasis, marked venous stasis disease, an old Charcot foot injury of his left foot and he stopped smoking at age 73. He has a family history of having a Protein S deficiency.
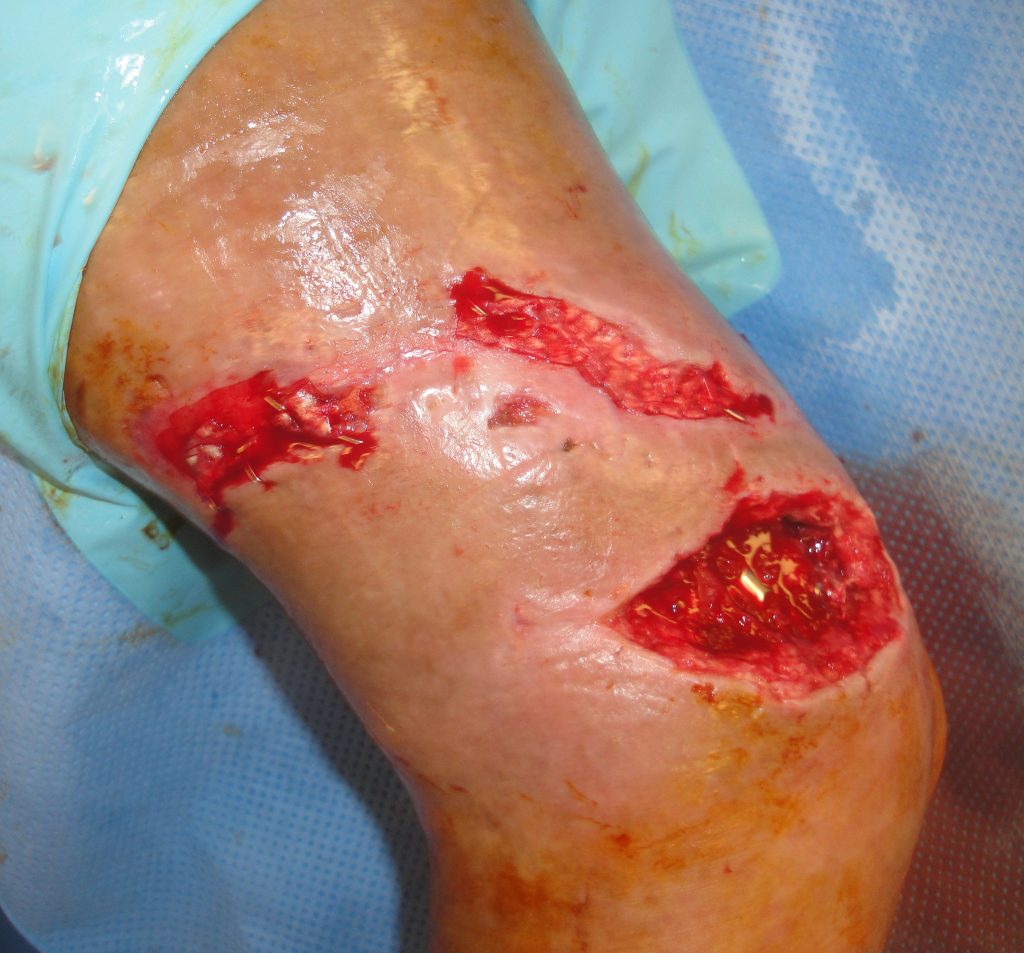
Fig.2. Open Ankle wound with exposed hardware plus proximal injuries
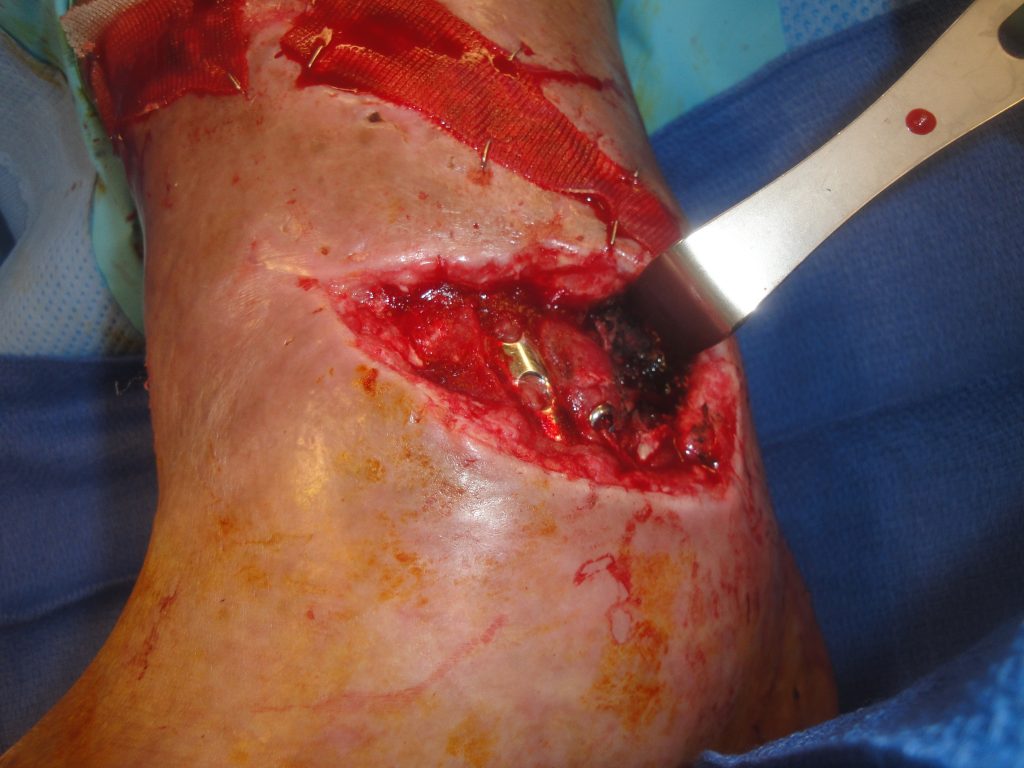
Fig.3. Open ankle wound with the degloving aspect demonstrated
Findings:
.The large full thickness medial right ankle wound was 12 cm. in length with exposed metal hardware, bone, tendons and had a degloving component extending around and down into the ankle joint. There was a 17 cm long oblique wound above the open ankle wound
Recent wound cultures were positive for Enterobacter cloacae, Bacteriodes fragilis & Diptheroids
Diagnosis:
Differential Diagnoses:
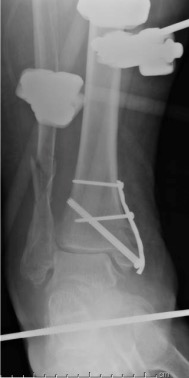
Fig.4. Initial Fracture Management
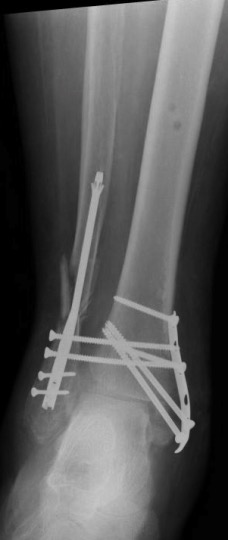
Fig.5. Reoperative Fracture Management
Workup Required:
Plan:
Expertise Needed:
Treatment:
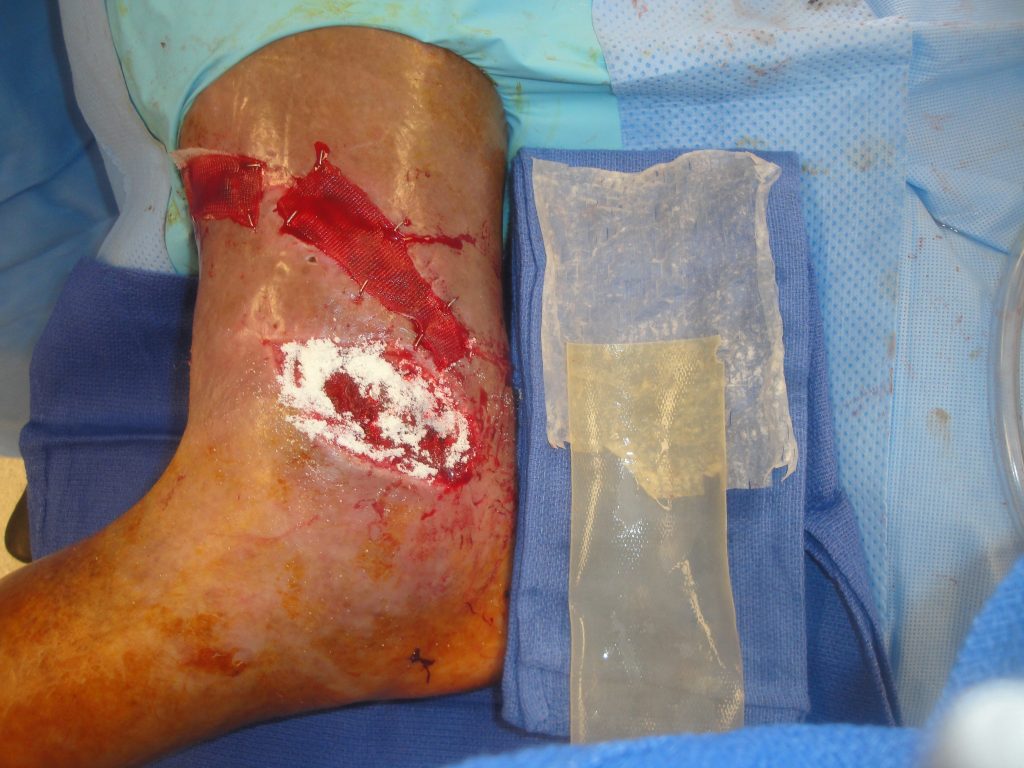
Fig.6. Open ankle wound with the UBM-ECM device to be utilized in management- the powder is already in place in the wound
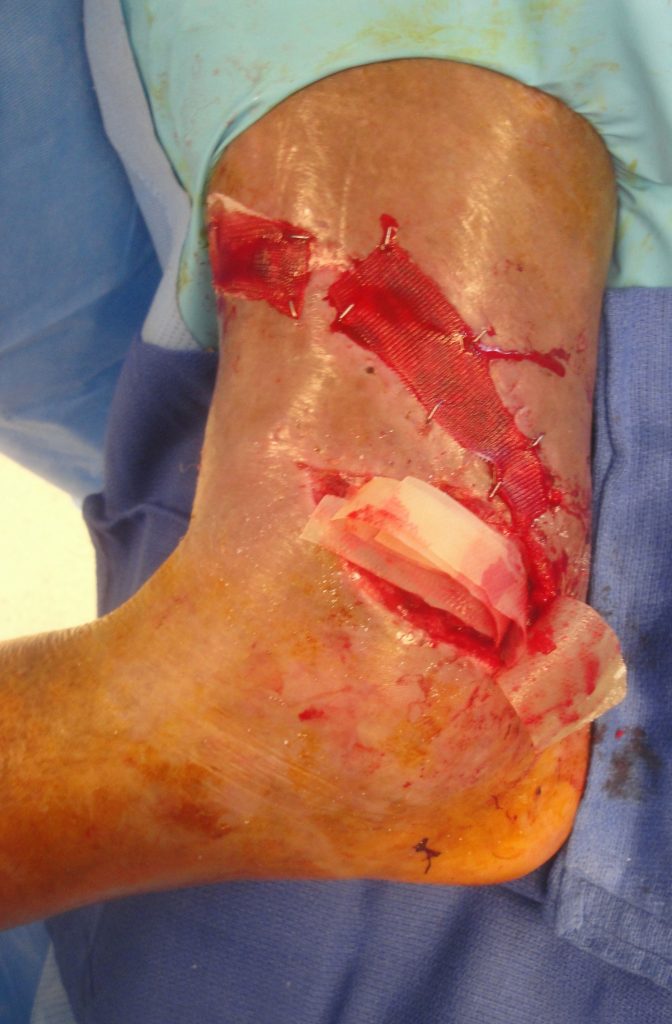
Fig.7. The lyophilized powder is now in the wound and multiple vacuum pressed sheets are to be stapled over this
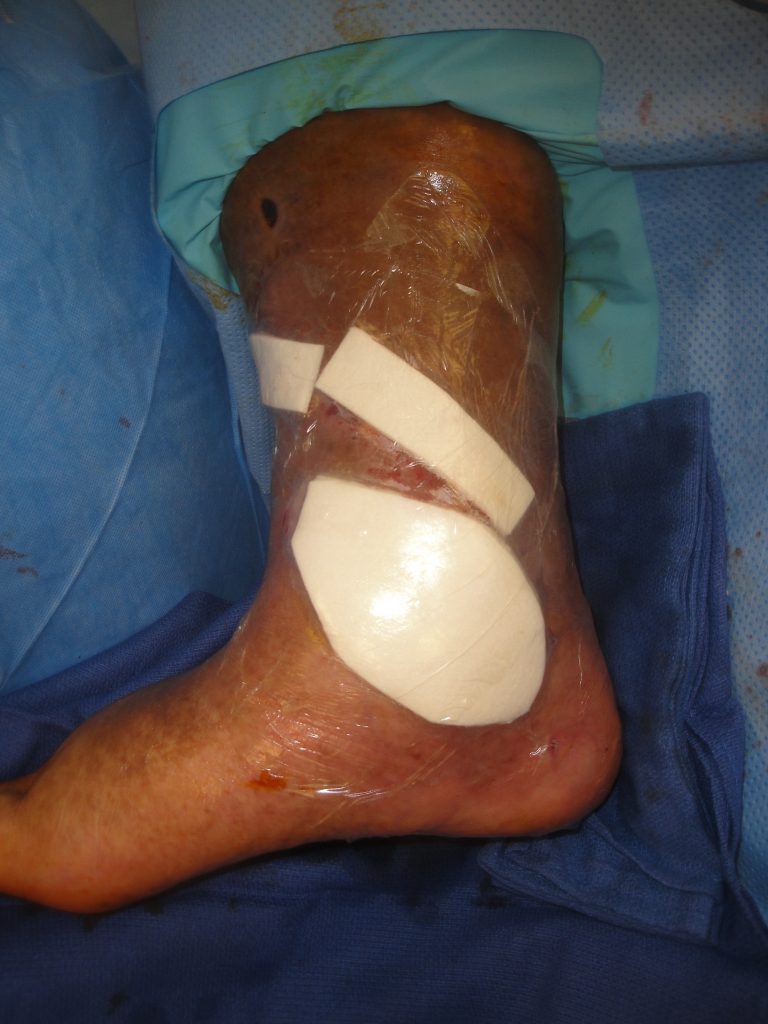
Fig.8. Secondary dressings in place to stent the UBM-ECM into the wounds.
Follow Up:
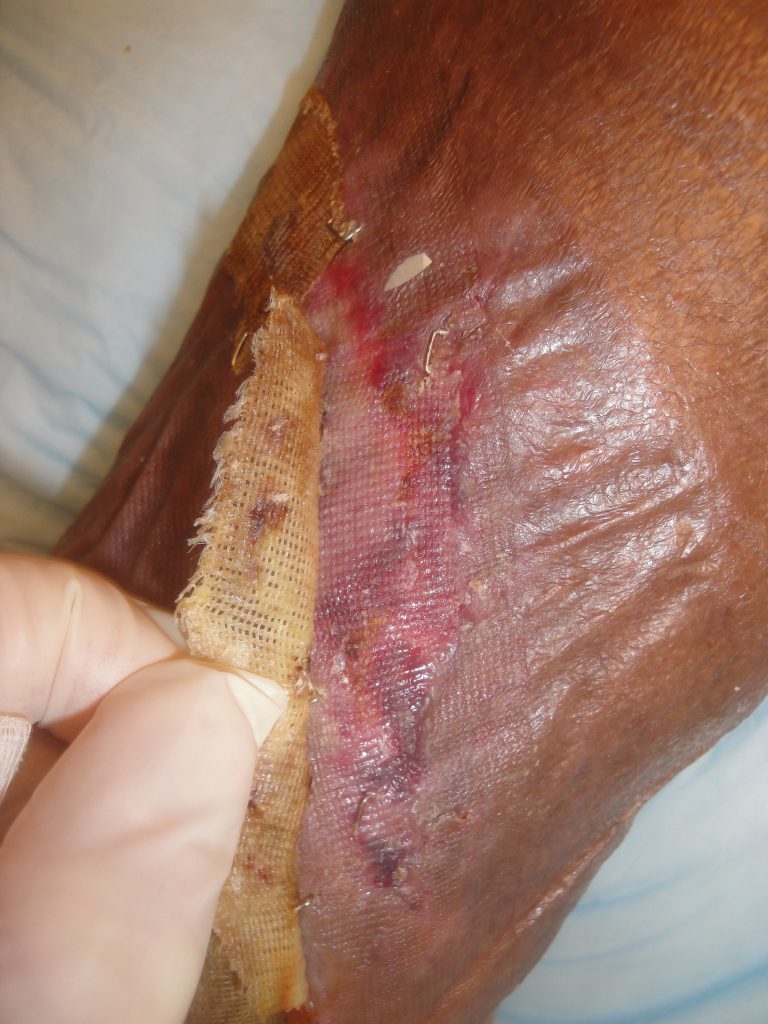
Fig.9. Upper wound healing at 3 weeks- Healed
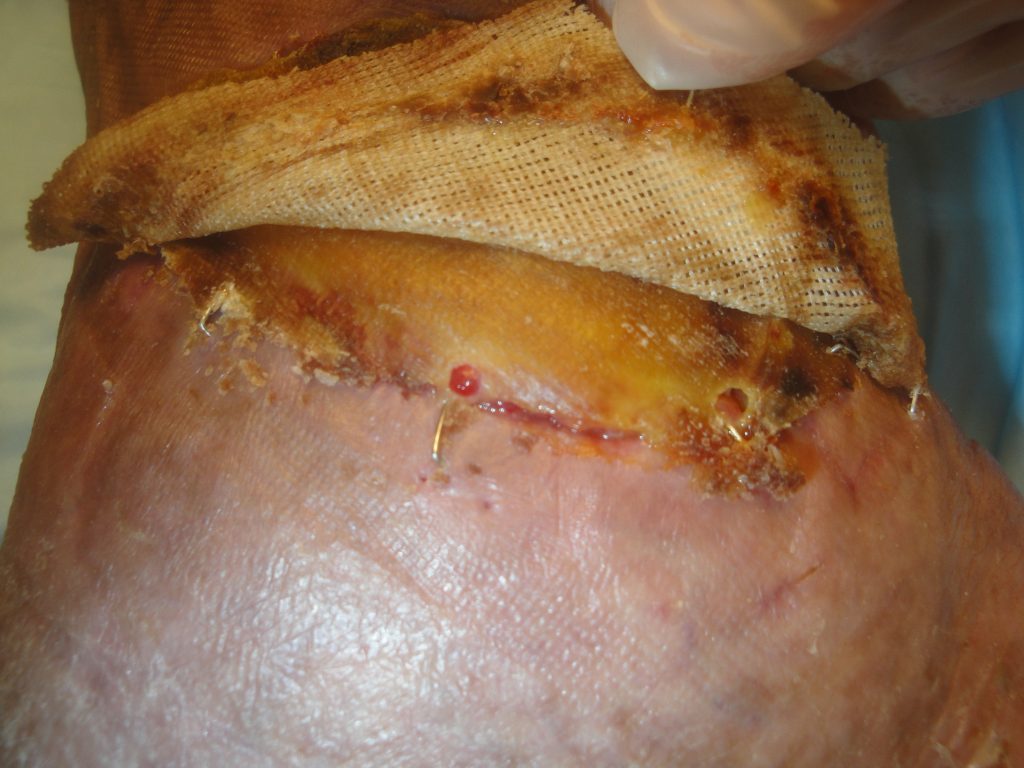
Fig.10. Open ankle wound healing at 3 weeks- UBM-ECM device adherent to the wound margin but overall too dry
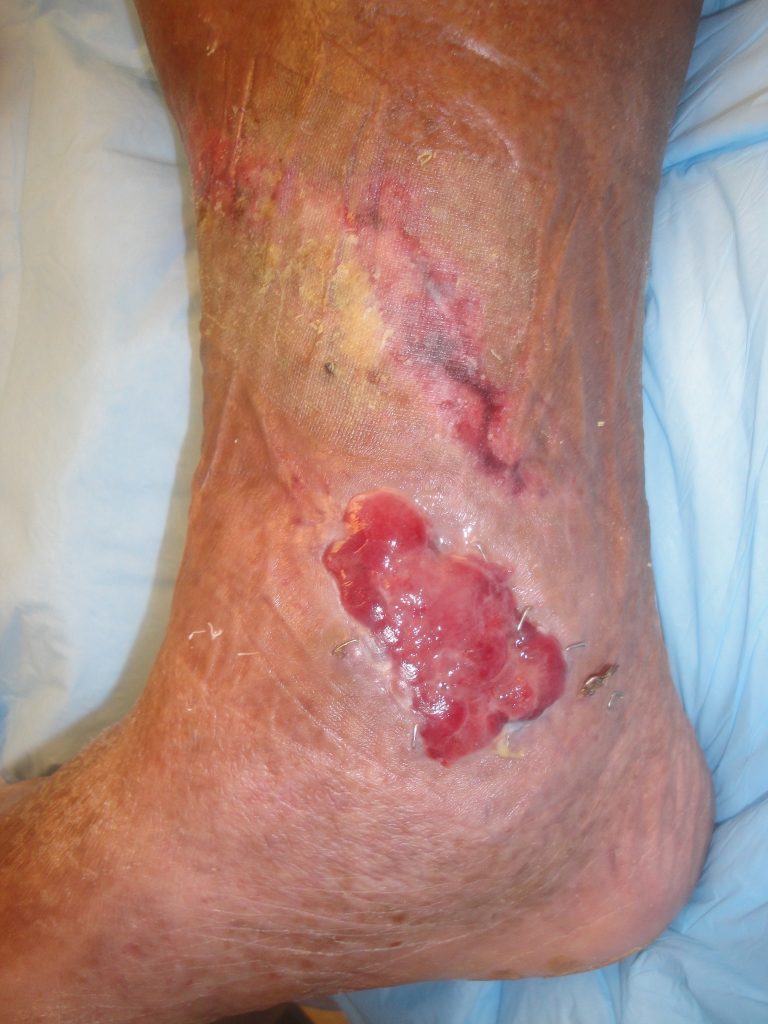
Fig.11. Right medial ankle wound 1 month later after daily hydrogel application
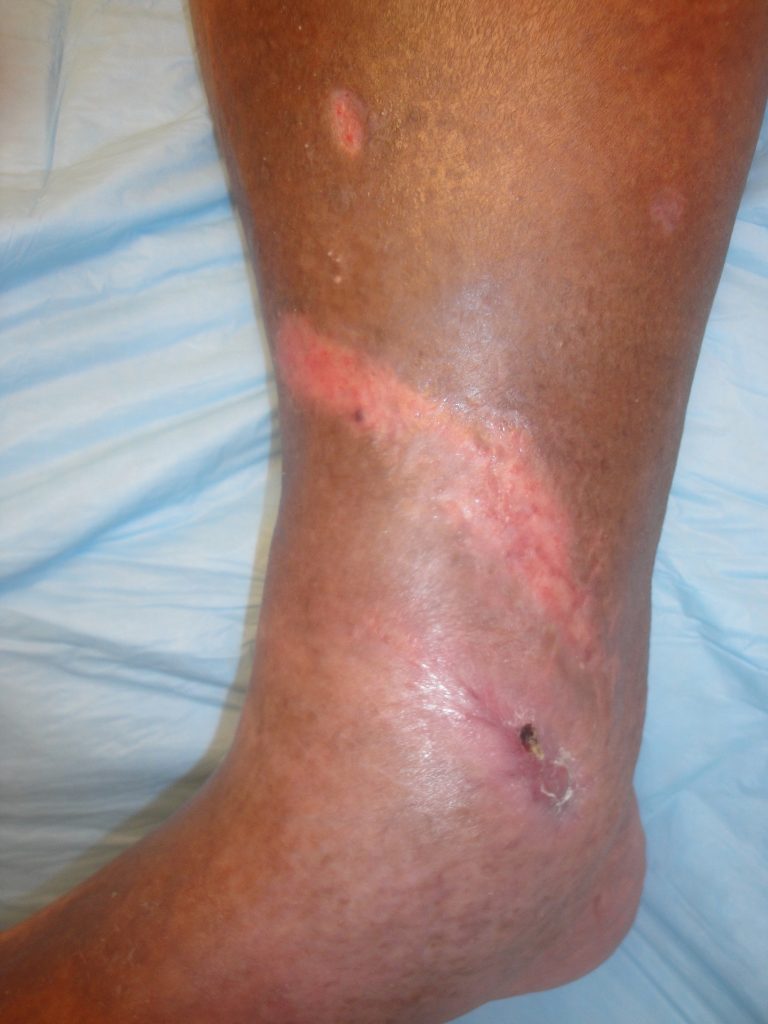
Fig.12. Right ankle wound appearance 4 months after UBM-ECM treatment- Total Healing with minimal scarring.

