Lumbar Wound from Liposarcoma Resection
History:
The patient is a 59 year old female diagnosed with right lower back liposarcoma with positive margin after resection. She first noted the mass approximately one year prior to presentation to plastic surgery. The mass grew and initial excision was performed six months later. This had a positive deep muscular margin and she was then referred to a tertiary cancer care center. She completed radiation therapy prior to re-resection. In conjunction with the surgical oncology team, the patient presented to plastic surgery for resection of margin with reconstruction. She is otherwise healthy, non smoker, and active.
Findings:
After tumor extirpation, the plastic surgery team was presented with defect 17 x 9.5cm defect through skin, subcutaneous tissue, fascia over lumbar region. The patient had extensive radiation changes to the surrounding skin and soft tissue [Figure 1].
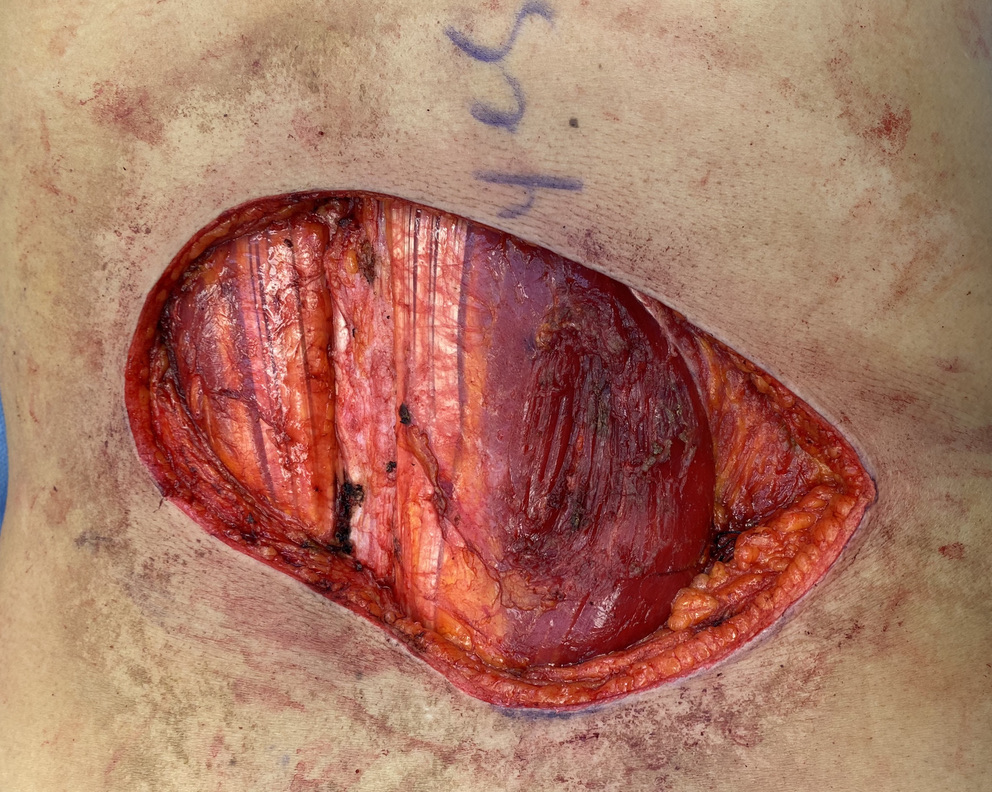
Figure 1. 17 x 9.5 cm defect through skin, subcutaneous tissue and fascia in lumbar region
Diagnosis:
Right lower back liposarcoma resection defect
Differential Diagnoses:
Workup Required:
Plan:
Expertise Needed:
Treatment:
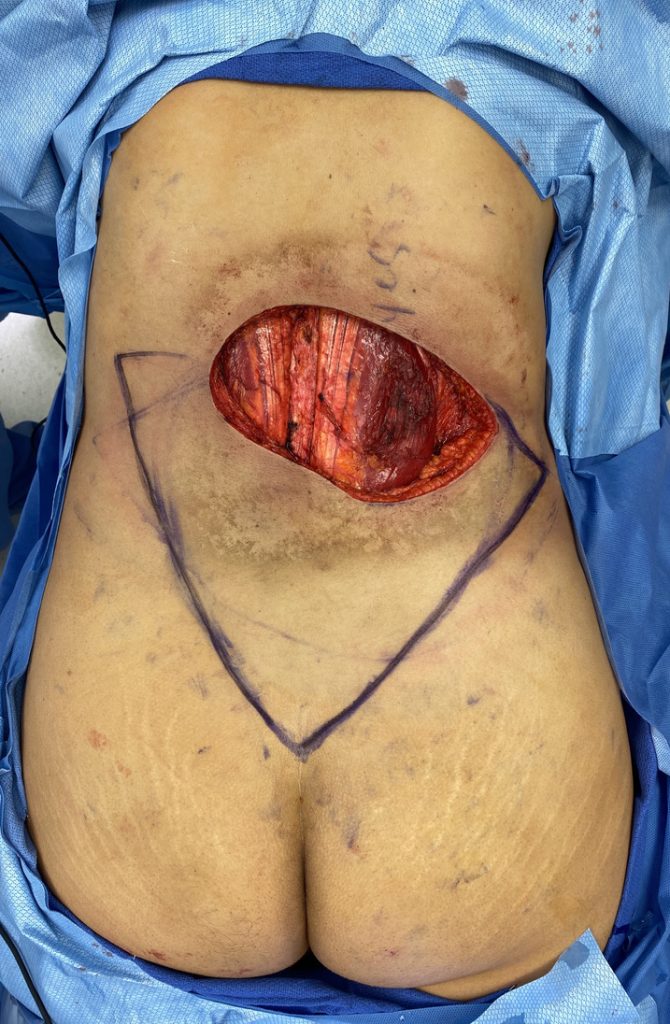
Figure 2. Flap design with double V to Y and three areas of advancement on bilateral flanks and gluteal cleft.

Figure 3. Flap dissection through skin, subcutaneous tissue and fascia. Lateral mobility is noted on bilateral flanks and superior gluteal area.

Figure 4. Demonstration of mobility of lateral segments for medial soft tissue coverage.
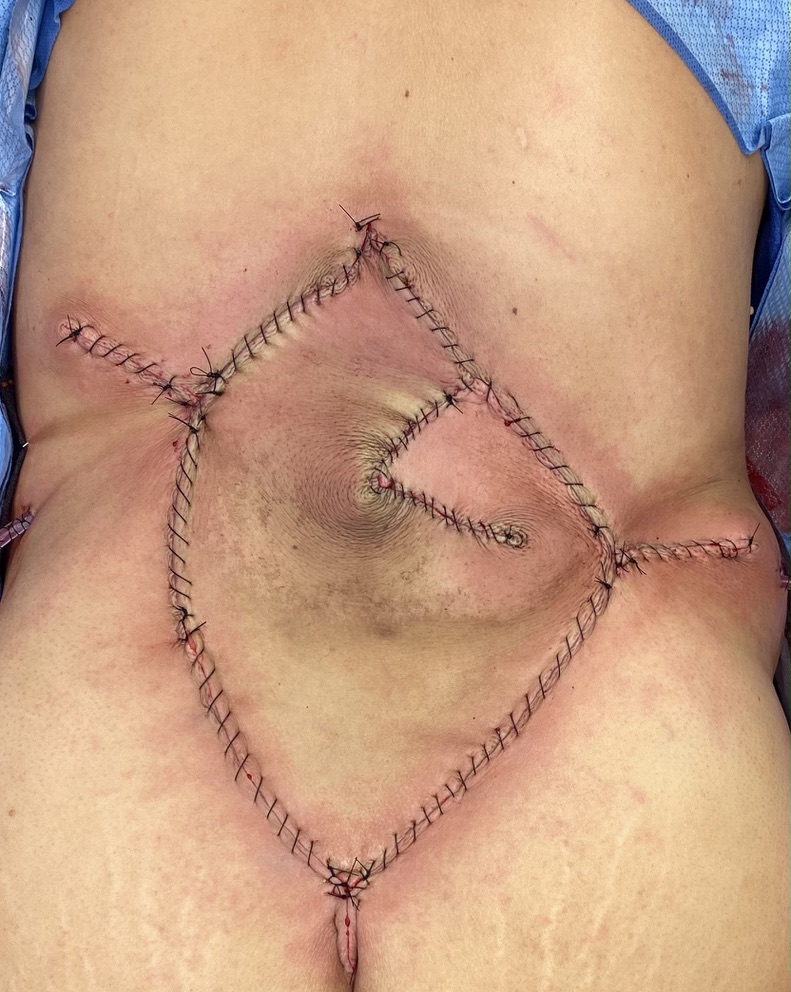
Figure 5. Immediate post operative result with double V to Y advancement with minimal tension closure in lumbar area.
Follow Up:
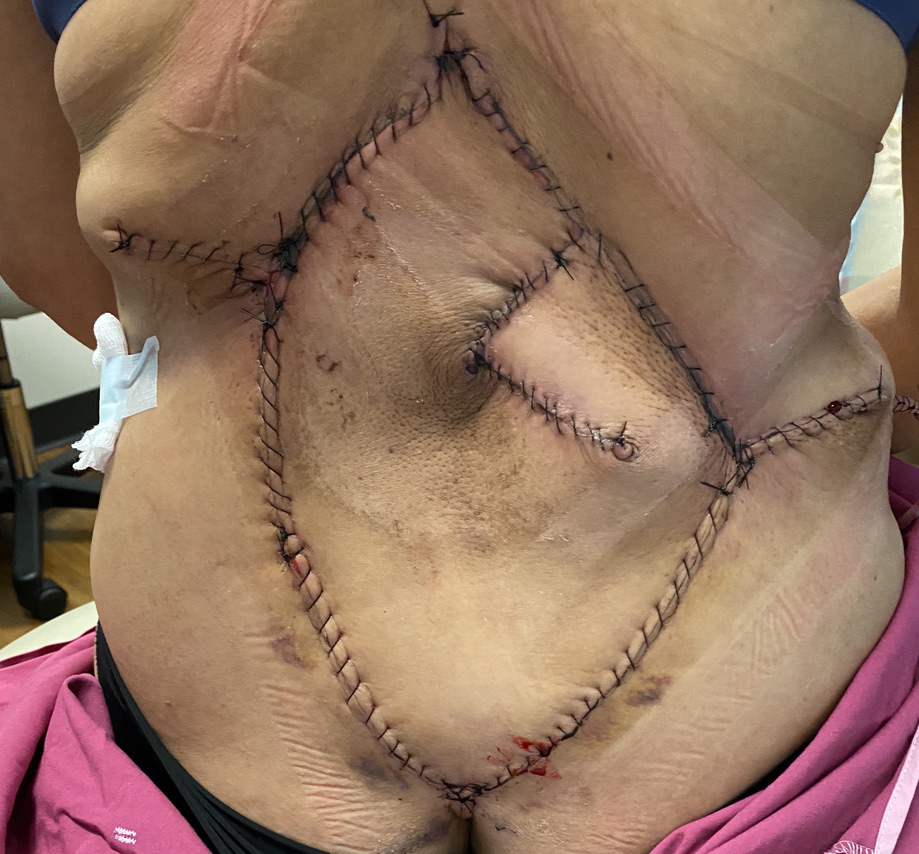
Figure 6. Post operative result at first follow up visit with well approximated incisions and no evidence of dehiscence, infection or drainage.
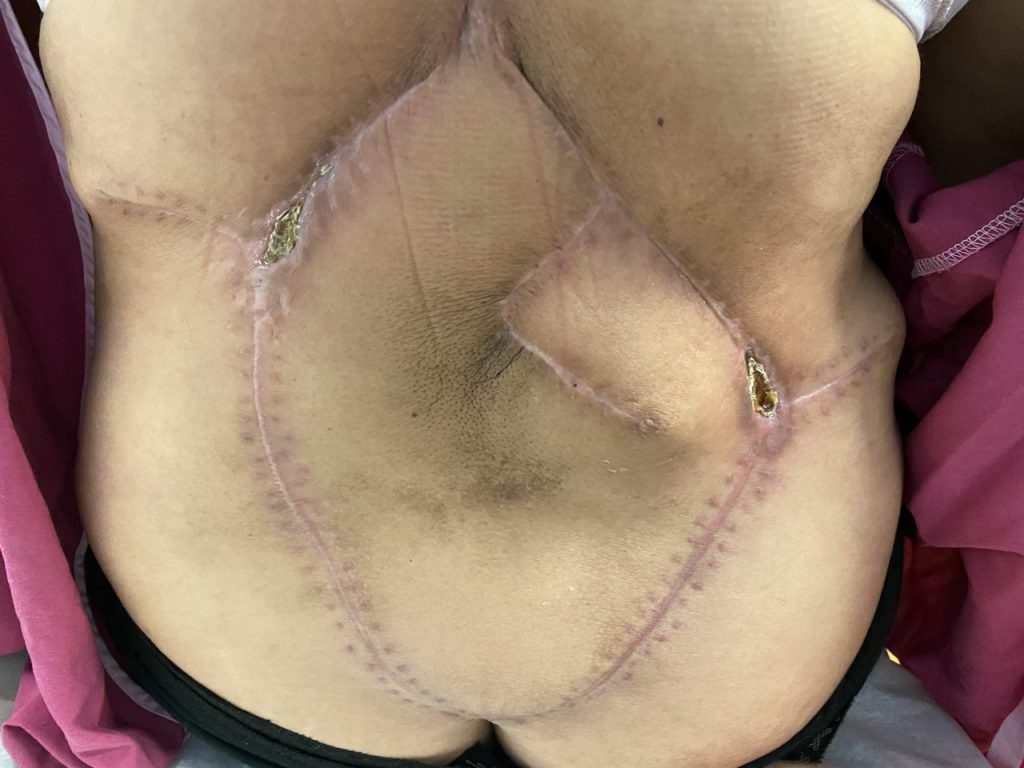
Figure 7. Two months follow up visit with well healed incisions and small areas of delayed wound healing at lateral T junctions

