Soft Tissue Avulsion Injury of lower leg
History:
Findings:
Soft tissue avulsion injury to medial left lower leg without any violation to muscle fascia or injury to tendon (Figure 1). Visible superficial vein that is intact but likely thrombosed. No active bleeding. Skin avulsion proximal mid and lateral lower leg (Figure 2).
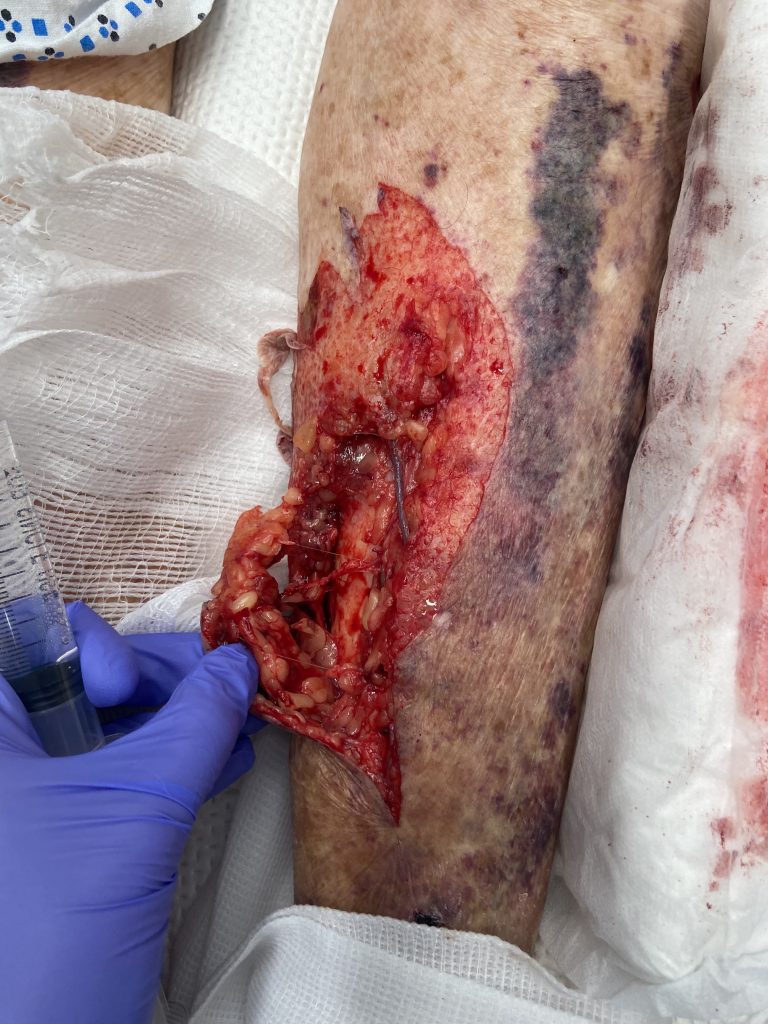
Figure 1: Soft tissue avulsion injury to medial left lower leg without any violation to muscle fascia or injury to tendon.
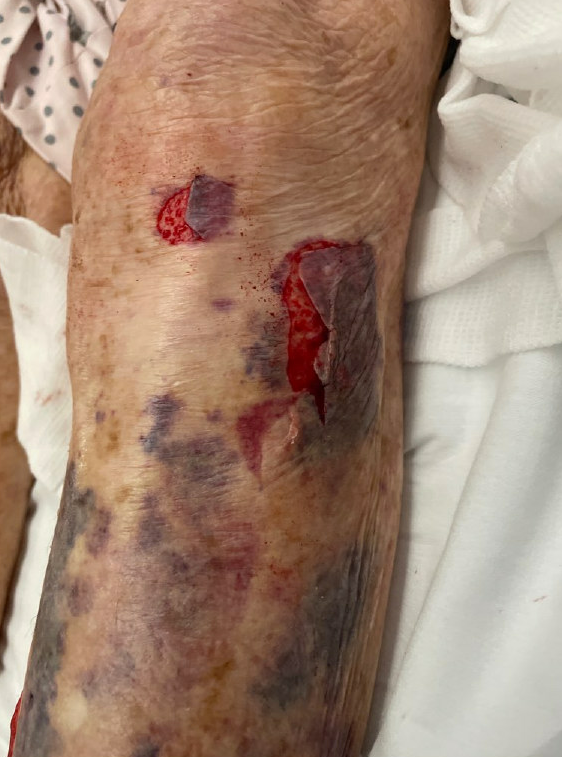
Figure 2: Skin avulsion injury to proximal mid and lateral lower leg.
Diagnosis:
Traumatic soft tissue avulsion injury to left lower extremity
Differential Diagnoses:
Workup Required:
Complete motor, sensory (tibial, superficial and deep peroneal nerve) and vascular exam (DP and PT pulse). LLE XR to rule out any osseous injuries.
-All were negative in this patient.
Plan:
Washout and partial closure in ED.
Expertise Needed:
Plastic surgeon.
Treatment:
Local field block achieved with 15cc of 1% lidocaine without epinephrine. Wound copiously irrigated with 1L NS mixed with Betadine. Soft tissue and overlying skin approximated distally with 3-0 chromic. Exposed superficial vein tied off with 3-0 Vicryl. Skin edges also approximated proximally. All areas of open wound were dressed with bacitracin and xeroform. Padded with gauze and wrapped with cast padding and ACE. Patient tolerated the procedure well.
-Discharge Instructions:
- Keflex for 1 week
- Keep dressing on for 2 days, followed by daily dressing changes with bacitracin/ xeroform/ kerlix and ACE wrap
- LLE elevation as much as possible
- Follow-up PRS clinic for wound check in one week.
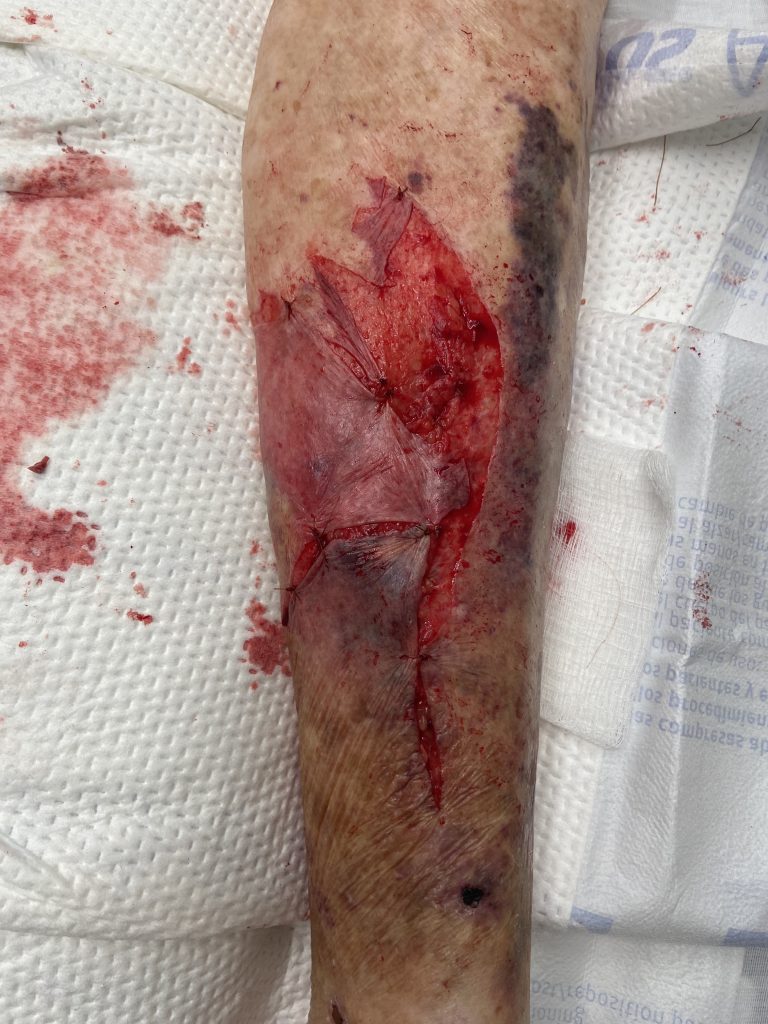
Figure 3: Immediately s/p wound wash out and partial closure.
Follow Up:
Patient was diligently followed up in PRS clinic every 1-2 weeks. Small fibrinous areas were intermittently treated with local debridement and/or silver nitrate. At the 3-month follow-up visit, the wound was closed secondarily with 4-0 Nylon without significant tension. 4-month post-injury, and wound continues to heal as noted in the photo below.
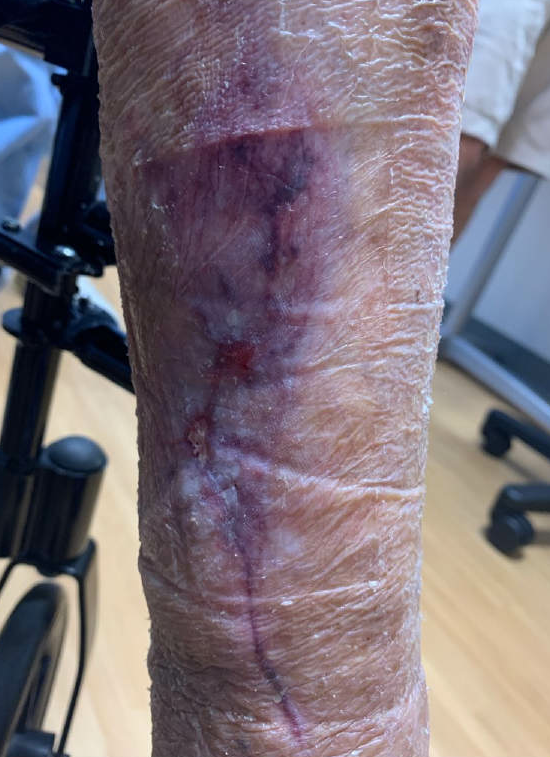
Figure 4: 4-month post-injury. Post-inflammatory skin changes with hyperpigmentation along initial laceration.
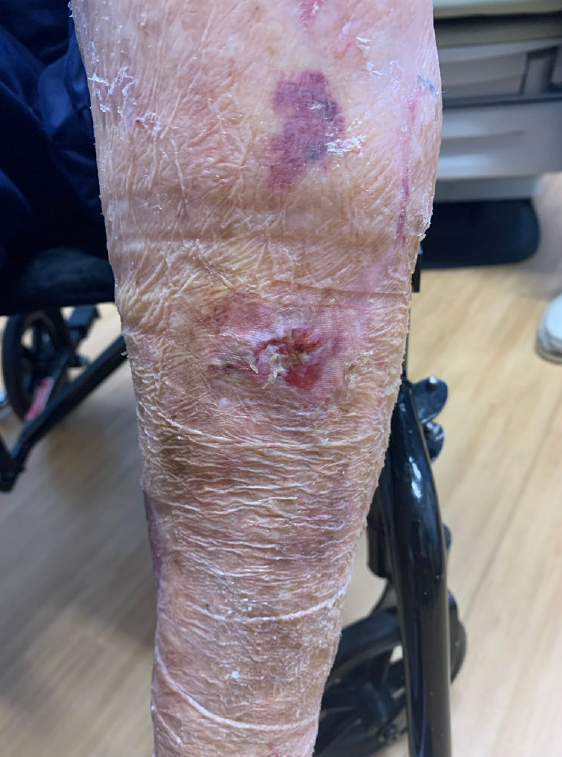
Figure 5: Well-healed prior superficial abrasion/ skin tear to left mid and lateral upper leg.

