Infected ischemic diabetic foot ulcer
History:
A 82-year-old woman with history of type 2 diabetes mellitus and percutaneous coronary intervention was referred to our university hospital with left infected foot ulcer. She kept walking because she didn’t feel any pain. She developed a small ulcer on lateral side of the left fourth toe when she stumbled one month ago. The wound became larger, her foot was swollen, and the IV toe became necrotic.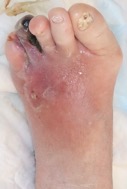
Findings:
Diagnosis:
Differential Diagnoses:
Venous leg ulcer, pressure ulcer, vasculitis, skin cancer, pyoderma gangrenosum
Workup Required:
- ABI, SPP for arterial flow
- Assessment of arterial flow with ultrasound, contrast CT, or MRA
- Culture from the deep area of the ulcer
- Laboratory test including inflammatory markers and HbA1c
Plan:
- Hospitalization
- Infection control by antibiotics and bed rest
- Revascularization
- Debridement
- Wound bed preparation
- Reconstruction
Expertise Needed:
Wound specialist, Wound nurse, Endovascular Surgeon, Vascular surgeon, Radiologist, Diabetologist, Ultrasound technician
Treatment:
After emergency hospitalization, culture from the deep area of the ulcer was taken and antibiotics treatment was started. Antibiotics was performed empirically fist and changed to the most sensitive one based on the culture results. ABI was 0.8 of right and 0.44 of left. Contrast CT and angiography revealed the arterial occlusion of common femoral artery (CFA).
After revascularization by endarterectomy of CFA, emergency debridement was performed and left the wound open. 7 days later, additional debridement was performed and applied Negative pressure wound therapy with instillation and dwell time;NPWTi-d ( 3M™ V.A.C. ®️ Ulta Therapy System; 3M). After 3 weeks, infection was completely controlled and wound bed preparation was completed. Mesh skin graft was performed and wound was healed without any complication.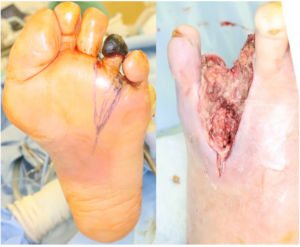
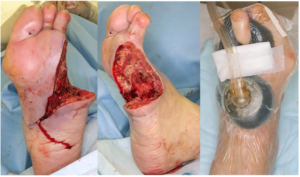
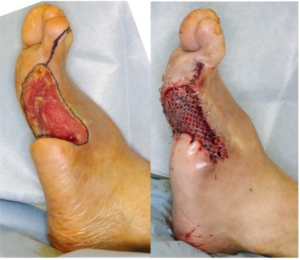
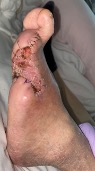
Follow Up:
After 2 years the wound had stayed healed and she could walk with custom made foot ware. There was no recurrence.

