Dorsal Hand Hematoma
History:
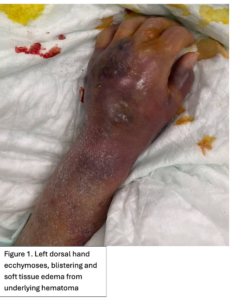
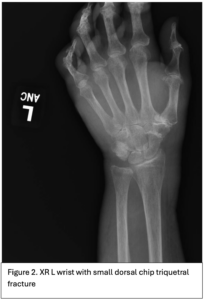
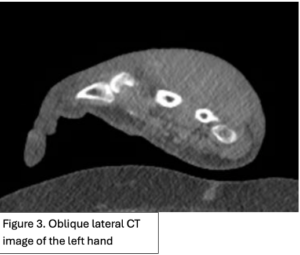
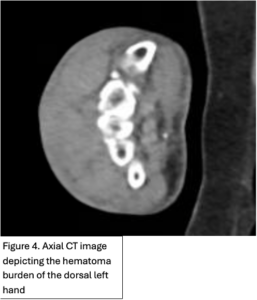
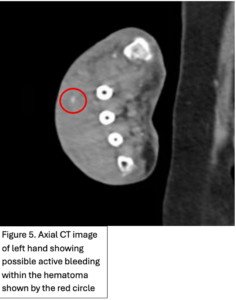
An 89-year-old right hand dominant female with dementia presented with significant swelling and bruising a left dorsal hand (Figure 1) after hitting the hand on a hand rail 10 days prior while being transferred to the bathroom at her nursing home. She has history of atrial fibrillation on Eliquis. Subsequently, the dorsum of her left-hand developed ecchymosis and became edematous. The patient was evaluated two days later at an out-patient facility where x-ray of the left hand showed no fractures or dislocations. The swelling and bruising continued to worsen and she was seen in the emergency department by the Plastic and Reconstructive Surgery team. A repeat 3V hand XR, 3V wrist XR, and CTA of the LUE were obtained, demonstrating a possible subtle dorsal chip avulsion from the triquetrum (Figure 2) and a dorsal hand hematoma (Figure 3 and 4) with a focal area of possible active extravasation (Figure 5) vs calcific density. She is a non-smoker.
Findings:
Figure 1. Left dorsal hand demonstrating significant soft tissue edema extending to tips of the digits. Ecchymosis of left first and fifth digits, dorsum of hand and wrist, and distal posterior antebrachium. Blisters evident on dorsum of left hand and between second and third digits. Figure 2. X-ray of the dorsal left hand and wrist demonstrating minimally displaced triquetral fracture. A subtle fracture through the dorsal edge of the triquetrum could not be excluded. Figure 3. and Figure 4. Illustrate the burden of the hematoma. Figure 5. Appreciates a focus of enhancement suggesting bleeding or possible dystrophic calcification, however with clinical correlation it was determined more likely to be an active bleed
.
Diagnosis:
Left dorsal hand hematoma
Differential Diagnoses:
Fracture, tendon or neuro-vascular injuries, abscess, cellulitis, isolated hand edema with superficial ecchymosis.
Workup Required:
X-rays of the left hand to (re)evaluate for fractures.
CT of left hand to evaluate for disruption of vascular integrity.
Plan:
Upon initial evaluation, non-invasive supportive measures and observation were considered. However, upon reexamination, the patient exhibited diminished sensation overlying the hematoma. The risk of ischemic compromise to the soft tissue and skin was elevated due to the underlying increased pressure, increasing potential for compromised tissue perfusion and subsequent necrosis. Consequently, a bedside incision, drainage, and evacuation procedure was recommended to mitigate the risk of skin loss, significant tissue defect, and the potential necessity for tissue flap reconstruction.
Expertise Needed:
Treatment:
The patient was positioned in a supine position. Local anesthesia was achieved by subcutaneous injection of 1% lidocaine with epinephrine into the skin over the hematoma. The hand was prepped with betadine and draped using sterile towels. A 4 cm skin incision was made over the hematoma cavity using a 15-blade scalpel. Blunt dissection with a curved clamp was performed to open the cavity. Hematoma fluid was expressed upon entry into the cavity. A curved clamp and digital examination were used to identify and disrupt any loculations within the cavity and express old hematoma debris. There was an active pulsating vessel noted which was suture ligated with a 4-0 Monocryl. The cavity was copiously irrigated using sterile saline. Hemostasis was ensured, and the cavity was subsequently packed with an epinephrine-saline wet-to-dry (WTD) dressing, wrapped with ABD pad, kerlix, and ACE wrap for compression.
The WTD dressing was changed twice a day during the patient’s admission.
Follow Up:
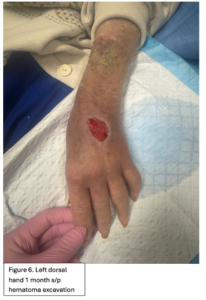
Examination at 1 month follow-up revealed a 3 x 3 cm healing wound of the dorsal aspect of the left hand with granulation tissue present in the base (Figure 6). There was no evidence of infection or exposure of vital structures such as the extensor tendons. The hand was neurovascularly intact. The patient endorsed intact sensation to the dorsum of the hand. There was marked stiffness appreciated on physical exam with significant swelling around the digits causing decreased range of motion. Integument was otherwise unremarkable. Daily Xeroform dressings were recommended for healing by secondary intention given the excellent granulation tissue already present at the superficial wound base (1). She was taken to hand therapy for edema control and range of motion exercises. She was instructed to follow-up in office 4 weeks later to re-evaluate wound healing progression and range of motion of the fingers.
Due to declining clinical condition as well as various social barriers, patient was initially lost to follow up and did not receive hand therapy. Hand therapy is imperative during recovery of hand injuries to aid in preventing joint contractures and maintain motion of the fingers. Examination at 6 month s/p hematoma evacuation showed a fully healed left dorsal hand, with a 5 cm scar (Figure 7.).


