Chronic Lower Leg Wound from osteomyelitis closed with Keystone perforator flap
History:
The patient is a 26-year-old female who presented to our plastic surgery team with a chronic left lower extremity wound. An original crush injury from a motor vehicle accident occurred about three years prior. Orthopedic procedures were done several times to repair original fractures, procedures complicated by hardware-associated infections, and incision and drainage procedures. The patient required multiple rounds of antibiotics, antibiotic spacers, and long-term suppressant doxycycline. The case is complicated by the patient’s past medical and social history of morbid obesity and tobacco use.
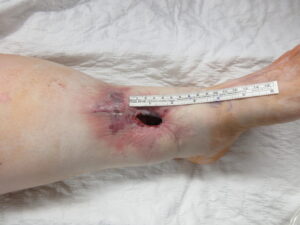
Figure 1. Pre-Operative Assessment of Left Lower Leg Wound. This is an approximately 5 x 3 x 3-centimeter open wound on the distal third of the left lower leg about 3 centimeters above the ankle. Surrounding erythema and edema is appreciated.
Findings:
Upon our consultation, orthopedic surgery performed a debridement and washout procedure followed by negative pressure wound therapy (NPWT). On examination, the patient had a 5 x 3 cm open wound involving the anterior distal third of the left lower leg about 3 centimeters above the ankle (Figure 1). The wound was about 3 centimeters deep and was clean-appearing with a small exudate area with possible bone exposure. Laxity of the skin around the ankle was observed, as it was imperative in order to use a keystone flap in reconstruction.1 Sensory and motor functions were intact throughout. There was a brisk capillary refill and palpable pulse of the dorsalis pedis artery.
Diagnosis:
Open wound of left lower leg secondary to poor wound healing with multiple failed medical and surgical interventions
Differential Diagnoses:
Osteomyelitis
Venous Ulcer
Arterial Ulcer
Vasculitis
Vasculopathy
Diabetic Ulcer
Workup Required:
Ankle-brachial index
Pulse volume recording
Computed tomography angiography
Standard preoperative labs
Plan:
Posterior tibial artery keystone flap with possible split-thickness skin graft and NPWT.
Expertise Needed:
Plastic surgery
Treatment:
The patient underwent wound debridement that included skin, subcutaneous tissue, muscle, and fascia of an area about 25 square centimeters down to the bone. Wound coverage was completed using the left posterior tibial artery perforator flap in a keystone fashion. This approach was selected due to its ability to spare major arteries and muscles, avoid the need for microsurgery, reduce operation time, and decrease hospitalization stay. Also associated with fewer complications, it was instrumental in this case where multiple comorbidities existed.2
A handheld Doppler was used to identify two perforator vessels along the middle part of the flap. To create the flap, the incision was made circumferentially in a keystone shape through the skin, subcutaneous tissue, and fascia, with the fascia being released circumferentially. The flap was freed of the tibia anteriorly. Superiorly and distally, the saphenous vein and posterior tibial artery were identified and protected. Dissection proceeded toward the defect, releasing the flap until the defect was reaching without any tension. Due to the amount of dissection performed, part of the flap was buried in the middle part of the defect following de-epithelialization. The area was irrigated with pulse lavage irrigation, and cultures were obtained.
The flap was inset superiorly with multiple interrupted 3-0 Prolene sutures. Appropriate bleeding of the skin edges of the distal portion of the flap was visualized. The flap continued to be approximated with multiple interrupted 3-0 Prolene sutures in a vertical mattress fashion. A 10 French round drain was placed along the medial part of the flap and exteriorized through a separate stab incision superiorly and was anchored with silk suture. The remainder of the flap was then inset. A handheld Doppler was used to identify vessel signals proximally and distally along the flap.
The donor site was partially approximated with staples with a small open area to decrease tension. Angiography with indocyanine green was performed, demonstrating excellent flap perfusion. Then, the temporary staples were removed, and the remainder of the flap was approximated with interrupted 3-0 Prolene sutures. A small open area remained along the donor site. A split-thickness skin graft was applied to the local flap donor site at a thickness of 0.014 inches. The skin graft was meshed in a 1.5/1 fashion and applied over the donor site, anchored with staples and interrupted chromic sutures. NPWT was applied as a bolster with good suction obtained, followed by appropriate wrapping.
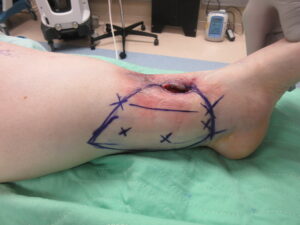
Figure 2: Flap Markings Drawn in the Operating Room Markings were made to create a keystone-shaped flap over the perforator vessels of the posterior tibial artery for wound coverage.
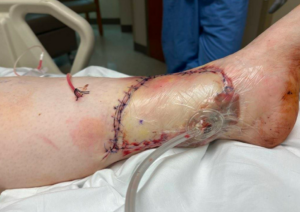
Figure 3A: Postoperative Assessment During Hospital Admission This shows the wound in the immediate postoperative period. The sutures are intact. Drain in place. Wound VAC is in place.
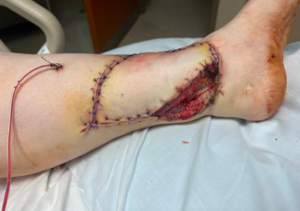
Figure 3B: Postoperative Assessment During Hospital Admission This shows the wound in the immediate postoperative period. The sutures are intact. Drain in place. Without wound VAC, demonstrating remaining open wound which was mesh grafted.
Follow Up:
Postoperatively, monitoring for potential complications was considered critical. While the patient was still admitted to the hospital, the wound was assessed on postoperative days one, two, three, four, five, six, and seven, with appropriate healing observed. Wound VAC was removed on post-operative day five. Three weeks postoperatively, the patient’s graft remained warm and pink. Staples around the skin graft were removed, and most sutures were removed around the flap except those at the medial border, where a small opening remained without any exposed structures. The drain was also removed at three weeks. The remaining sutures were removed at five weeks. We continued to follow up at seven, nine, and fourteen weeks without any complications.
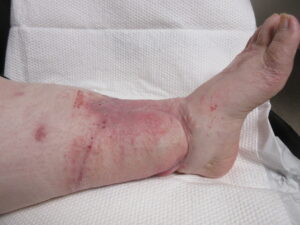
Figure 4A: Fourteen Week Postoperative Assessment Anterior-medial view of the flap.
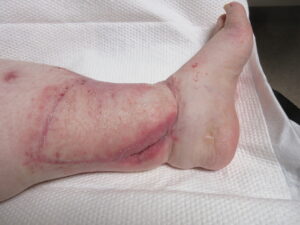
Figure 4B: Fourteen Week Postoperative Assessment. Medial view of the flap showing donor site area healed by skin graft and secondary intention.

