Traumatic Hematoma–Related Leg Ulcer of the Left Lower Leg in a Nonagenarian on Anticoagulation
History:
A 93-year-old woman with chronic atrial fibrillation on apixaban, hypertension, hyperlipidemia, CKD3a, HFpEF, glaucoma, and bilateral hip and left knee arthroplasties presented with a worsening wound on the left lower leg. Baseline functional status was independent of family support. She had no history of diabetes, PAD, chronic venous insufficiency, or prior ulcers.
On 9/11/2025, she sustained blunt trauma to her anterior left lower leg while exiting a bathtub, initially causing minor bleeding that rapidly worsened once the leg was lowered. In the ED, a large tense hematoma was noted. Due to active bleeding while anticoagulated (apixaban), she received Kcentra before being scheduled for surgery.
On 9/15/2025, she underwent operative washout and hematoma evacuation by surgery, and staple closure. After the hematoma was evacuated she was found to have a degloving injury with separation of the skin and the subcutaneous tissue. Her skin was very thin, so the surgeon closed it with interrupted staples, with the length of the incision being 17cm. She also had a JP-drain placed subcutaneously. Skin graft was forgone due to the patient’s thin and fragile donor sites. She progressed to full weight-bearing postoperatively and was discharged to short-term rehabilitation with daily Xeroform, gauze, and Kerlix dressings.
Her anticoagulation was resumed on 9/16/2025, but on 9/17/2025, she was readmitted for fatigue, dyspnea, and rectal bleeding due to her anticoagulation being resumed. She was diagnosed with COVID pneumonia and Enterococcus/Citrobacter UTI requiring ICU care. During this stay, her hemoglobin remained stable, and apixaban was continued without further bleeding. The surgical incision remained intact. Wound care was transitioned to daily Hibiclens cleansing, collagen hydrogel, Adaptic, ABD pads, and light compression.
At surgical follow-up on 10/7/2025, staples were removed, and non-adherent eschar was debrided, and she was referred to the wound center for ongoing management.
At her initial wound center visit on 10/24/2025, she had developed a large anterior-lateral ulcer at the prior hematoma site with exposed subcutaneous fat, biofilm, and yellow slough. She denied wound pain or systemic symptoms. On 10/30/2025, she was accompanied by her daughter to her wound physician evaluation and remained asymptomatic and stable on her anticoagulation. She currently lives at home and receives PT/OT. This presentation is consistent with reported post-traumatic hematomas in elderly anticoagulated patients2.

Figure 1. Post-hematoma necrosis of the skin of the antero-lateral left leg, showing evolving hematoma-related skin breakdown after operative washout and closure (9/17/2025). There was no sign of wound infection or cellulitis, the incision site was well approximated. At this point no debridement was done.
Findings:
On serial examination, the patient appeared comfortable with stable vital signs (e.g., 12/4/2025: BP 124/75 mmHg, pulse 73 bpm, temperature 98.2°F). Cardiopulmonary exams were normal. Dorsalis pedis pulses were +2 bilaterally, and the foot was warm with good capillary refill. Edema present early in the treatment course resolved completely with compression.
Wound Examinations
10/24/2025 (Initial wound center evaluation)
- Large anterior-lateral ulcer
- Rolled edges, thin biofilm, yellow slough
- Small serosanguineous drainage, no odor
- No erythema, warmth, or induration
- Full-thickness ulcer with exposed subcutaneous fat, and no infection
- Measurements: 18 × 8.3 × 0.2 cm (149.4 cm²)
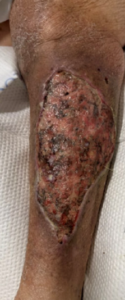
Figure 2. Full-thickness ulcer with exposed subcutaneous fat, rolled edges, and biofilm/slough prior to debridement (10/24/2025).
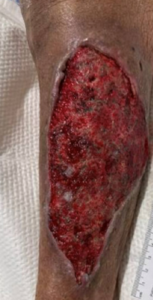
Figure 3. Post-debridement wound (18 × 8.3 cm), showing a cleaner, granulating bed with exposed fat and controlled drainage (10/24/2025).
On 10/28/2025, post-debridement, the wound was evaluated by a plastic surgeon for a split-thickness skin graft. The wound was clean, with no signs of necrosis, and the measurement remained unchanged from the last observation. The base of the wound was subcutaneous tissue, predominantly fatty tissue, with some interspersed granulation tissue. The plastic surgeon decided not to do the split-thickness skin graft (STSG) because it would create two wounds that are about the same size and could lead to prolonged immobilization, due to her fragile skin, which could make the donor site difficult to heal. These two wounds would increase her immobility, making it harder for her to heal. Her treatment at the time consisted of Hydro-fera blue, followed by dry gauze, ABD, and a compression bandage. The surgeon referred the patient to the wound center for follow-up treatment.
10/30/2025 follow-up at the wound center, the wound was treated with Medical grade honey, alginate, and light compression, and showed early epithelialization and resolved edema.

Figure 4. Wound progress showing early epithelialization and resolved edema (10/30/2025).
Over the 4-week treatment period (11/06/2025–12/11/2025), the wound demonstrated Increased red/pink granulation, reduced slough, and early epithelialization. It showed large, creamy, serous/serosanguineous drainage, rolled, fixed edges, peri-wound ecchymosis, and early scarring. Her Edema had fully resolved, and her wound was visibly cleaner and contracting.
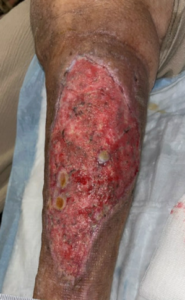
Figure 5. Wound size 17.4 × 8.6 × 0.2 cm (117.53 cm², 15.67 cm³), demonstrating increased pink granulation tissue, reduced slough, and visible contraction (11/6/2025).
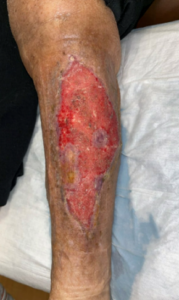
Figure 6. Wound appearance under Thera-Honey and two-layer light compression, showing new skin islands within the wound bed and flattening of the edges (11/20/2025).
On 12/04/2025, her wound exhibited persistent red-pink granulation and significant epithelialization, with large but benign serosanguinous drainage. The wound showed Flattening edges with multiple epithelial islands, no edema, cellulitis, or pain, and 50% area reduction and >75% volume reduction.

Figure 7. Wound size 13 × 5.5 × 0.1 cm (56.16 cm², 3.74 cm³), with significant contraction, large areas of epithelialization from the edges and centrally, minimal slough, and no leg edema (12/4/2025).

Figure 8. Wound showing continued contraction, advancing epithelialization, and further reduction in wound depth and surface area (12/11/2025).
Imaging
Left Tibia/fibula X-ray (9/17/2025)
- Postoperative changes of left TKA
- Surgical staples and soft tissue edema
- No fracture or bony injury
Normal prosthesis alignment
Diagnosis:
Traumatic hematoma associated full-thickness ulcer of the left lower leg with exposed subcutaneous fat in an elderly patient on chronic anticoagulation.
Diagnosis was based on the trauma → hematoma → necrosis sequence, absence of peripheral arterial disease, intact distal perfusion, and progressive improvement with standard wound care.
Differential Diagnoses:
- Venous leg ulcer
- Mixed arterial/venous ulcer
- Anticoagulant-associated soft tissue necrosis
- Pressure-related necrosis
The absence of venous stasis changes, lack of undermined violaceous borders, steady healing trajectory, and regular pulses made atypical causes unlikely.
Workup Required:
- Vascular assessment (DP/PT pulses, limb temperature, edema)
- Left tibia/fibula radiograph to rule out fracture
- Serial monitoring for local infection
- ABI or duplex ultrasound to be performed to rule out venous insufficiency.
Plan:
Management was guided by Wound Healing Society chronic wound care guidelines. ¹
- Serial sharp and mechanical debridement to remove necrotic hematoma tissue.
- Maintain moist, antibacterial wound conditions.
- Use light compression to manage edema while maintaining perfusion.
- In this age group of patients on anticoagulation weigh the risk vs benefits of creating an extra donor site wound with spilt-thickness skin graft.
- Consider the risk of prolonged immobility.
- Regular wound center follow-up with visiting nurses at home if needed
- PT/OT to preserve mobility and reduce fall risk.
- Education on nutrition, leg elevation, and activity modifications.
- Continue apixaban with close coordination between wound care, surgery, and cardiology.
Expertise Needed:
- Wound care physician
- Wound-trained nursing staff for dressing management and compression
- General/vascular surgery for initial hematoma evacuation; available for grafting if required
- Physical and occupational therapy for mobility and fall prevention
- Primary care/cardiology for anticoagulation oversight
Treatment:
Initial Surgical Treatment (9/11/2025)
- Kcentra reversal of apixaban
- Operative washout and hematoma evacuation
- Staple closure
- Daily Xeroform, gauze, and Kerlix dressings at STR
Hospital Readmission (9/17/2025)
- Daily Hibiclens cleansing
- Collagen hydrogel + Adaptic + ABD pads
- Light Coban/Ace compression
- Frequent dressing changes 3x per week and outpatient follow-up
Wound Center Course
Frequency of Wound dressing:
Frequency should be adjusted based on the wound’s improvement. For the first six weeks, when the wound had intense drainage, wound care frequency was three times a week due to heavy drainage. This initial frequency of wound care was once weekly at the wound center and twice weekly at home by a visiting nurse.
By 11/06/2025: When the wound had minimal drainage, signs of new epithelization, and the wound bed was clean, the frequency of wound care was changed to once weekly due to minimal drainage, and all wound care was performed at the wound center after 11/06/2025.
Excisional Debridement (10/24/2025)
Serial sharp and mechanical debridement were performed in accordance with wound bed preparation principles3.
- 18 × 8.3 cm ulcer with 100% necrotic tissue
- Excisional debridement of subcutaneous tissue size was 149.4 cm²
- Depth increased to 0.2cm post-debridement
- Immediate improvement in wound bed quality with minimal bleeding
Initiation of Honey-Based Therapy (10/30/2025)
- Mechanical debridement with Vashe and gauze to remove loose biofilm/slough
- Medical grade honey + alginate + protective pad over wound
- Light compression with two layer compression system on the whole lower leg including ankle
Early Improvement (11/6/2025)
- Mechanical debridement
- Continued medical grade honey + alginate + light compression
- Increased granulation and contraction
Transition to TheraHoney and Two-layer compression (11/20/2025)
- TheraHoney sheet + dry protective dressing
- Two-layer light compression
- Reinforced leg elevation, nutrition, and signs of infection
Rapid Healing Phase (12/4/2025)
- Mechanical debridement of bioburden
- Continued TheraHoney + two-layer compression
- No edema or pain and marked reduction in wound size
Overall treatment plan:
- No systemic antibiotics were required
- No signs of cellulitis or infection occurred
- Anticoagulation was safely maintained
- Mobility was preserved with PT/OT
- Wound care focused on reducing biofilm burden with gentle mechanical debridement and edema control with two-layer compression and dressings to provide moist wound healing.
Follow Up:
Over the 6-week treatment period (10/24/2025–12/4/2025), the wound demonstrated substantial improvement, with the wound bed covered by nearly 40 percent epithelization. The wound developed robust granulation and epithelialization, and complete resolution of edema with light compression. She had no wound-related pain, enabling continued mobility and rehabilitation. She required no skin grafting or advanced biologic therapy, and she had no recurrence of bleeding while on anticoagulation with apixaban. Her wound Surface area decreased from 149.9 cm² to 56.16 cm² (>50% reduction).

Figure 9. The patient continued weekly follow-up at the wound center, with excellent progress and ongoing epithelialization (12/04/2025).
At extended follow-up on 01/08/2026, the left lower leg ulcer demonstrated sustained contraction and advancing epithelialization without evidence of infection, edema, or recurrent hematoma more than three months after initial wound center presentation, consistent with ongoing progression toward complete closure (Figure 10).
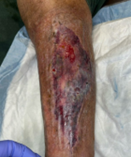
Figure 10. Extended follow-up demonstrating durable healing (1/08/2026).
As epithelialization progressed, aggressive wound care was de-escalated. On 1/15/2026, treatment transitioned to petroleum-based gauze to maintain moisture over the remaining open area with continued two-layer compression. During her visit on 1/22/2026, the wound had sufficiently epithelialized to permit transition to twice-daily moisturizer application to the entire wound and to a mild compression sleeve worn only during the day (Figure 11).
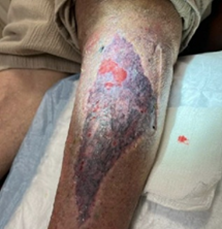
Figure 11. Late wound healing and epithelization (1/22/2026).
At final follow-up on 1/29/2026, the wound was completely healed. The patient was advised to continue routine skin moisturization to prevent dryness and to wear a mild compression sleeve during daytime hours for one additional week to prevent recurrence (Figure 12).
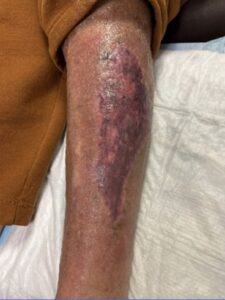
Figure 12. Complete epithelialization and wound closure (1/29/2026).

